AIG: Improper (but Logical) Med-Legal Underpayment

AIG improperly reduced a California Medical-Legal bill by 88%, providing a dramatic example of how California law incentivizes payers to incorrectly reimburse physicians who treat injured workers.
Rather than properly reimbursing a Qualified Medical Evaluator (QME) for a supplemental report, AIG seemingly used a profits-first calculus that takes into account the utter lack of consequences payers face when breaking the rules. Below, we document AIG’s victimization of a physician evaluator who did exactly what was requested of them.
Why do payers like AIG remit erroneous reimbursements to physicians? Incorrect reimbursements make logical sense.
- California law allows the payer to retain the provider’s reimbursement, if the provider fails to properly submit a timely Second Review appeal to dispute the erroneous payment amount.
Why do many payers simply deny a provider’s Second Review appeal for correct reimbursement? It makes logical sense to deny these appeals.
- California law allows the payer to retain the provider’s reimbursement, if the provider fails to subsequently pay $180 to file for Independent Bill Review (IBR).
The reimbursement-reducing steps taken by AIG perfectly represent how California law incentivises payers to (logically) ignore reimbursement rules and (logically) underpay California workers’ comp physicians. In this AIG example of improper reimbursement, if the QME fails to submit either the Second Review or the IBR, California law allows AIG to keep the QME’s reimbursement.
QME Requested to Review 2,698 Pages of Records
In May 2021, a party to an AIG liability dispute requested the QME to review 2,698 pages of records and issue a Supplemental Medical-Legal Evaluation report.
Effective April 1, 2021, the new MLFS directs payers to reimburse physician-evaluators $3 per page of records reviewed. Further, the new MLFS instructs that when a party sends records to the medical-legal evaluator for review, the sender of records must include an attestation confirming an accurate page count for the records:
Any documents sent to the physician for record review must be accompanied by a declaration under penalty of perjury that the provider of the documents has complied with the provisions of Labor Code section 4062.3 before providing the documents to the physician. The declaration must also contain an attestation as to the total page count of the documents provided. [emphasis added]
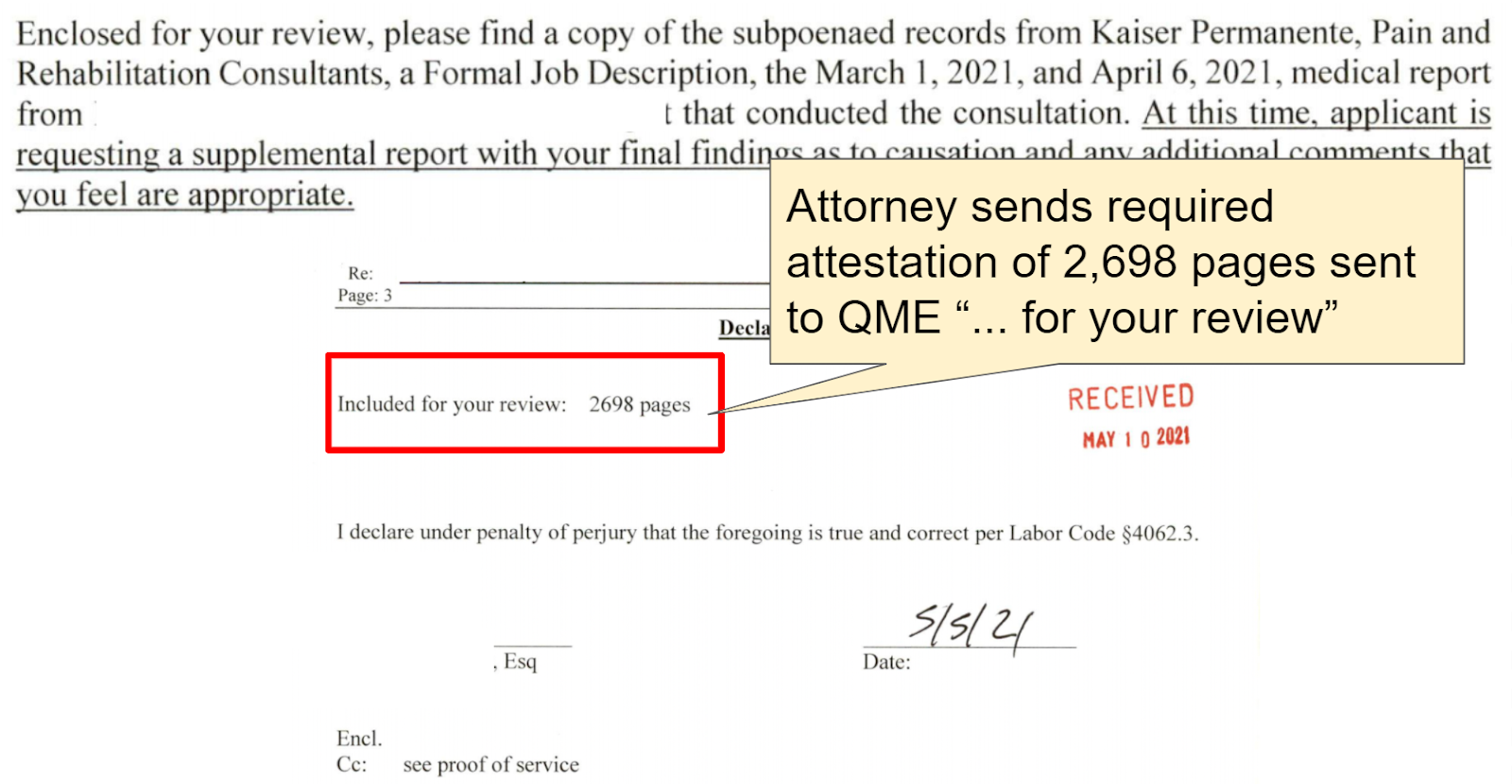
Below is the request sent to the QME for the Supplemental Medical-Legal Report, and the required attestation specifying the number of pages sent for review as 2,698:
QME Submits 70-Page Supplemental Evaluation Report
As requested, the QME reviewed the records and sent both parties a 70-page report. The physician submitted a bill to AIG for the evaluation report (code ML203) and and for the review of records (code MLPRR).
When reimbursing for a Supplemental Medical-Legal Evaluation, the new MLFS instructs that the reimbursement for ML203 includes 50 pages record review. Since the records sent for review exceed 50 pages, AIG owes the physician reimbursement of $3 for each additional page.
Therefore the physician’s bill reports code MLPRR for 2,648 units, or pages, of record review:
AIG Attempts to Evade Proper Reimbursement
In response to the physician’s bill, AIG sent the physician an Explanation of Review (EOR) that incorrectly reflects only 265 page units for MLPRR, rather than the 2,648 page units the physician’s bill actually reported.
The total reimbursement for record review as billed is $7,944.00 But using their incorrect 265 page unit count to calculate reimbursement, AIG decided to allow the physician just $795 in reimbursement after reviewing 2,648 pages of records. The EOR neither acknowledges the reduction in pages, nor offers any explanation or reasoning.
AIG Applies PPO Discount to Med-Legal Bill
AIG improperly reduced reimbursement even further by applying a PPO reduction. As the EOR shows, AIG took an additional $411.75 MultiPlan PPO discount, including $292.50 off the primary billing code ML203, and $119.25 off the fraction of MLPRR units AIG elected to pay:
We’ve said it before (recently), and we’ll say it again: claims administrators may not apply PPO or other network discounts to bills for Medical-Legal services.
According to the Division of Workers’ Compensation (DWC), Labor Code Section 5307.6 governs the MLFS. Therefore, discount arrangements under the Official Medical Fee Schedule (OMFS), governed by Labor Code Section 5307.1, are not allowed.
AIG may have missed this memo — along with the DWC Newsline and Independent Bill Review (IBR) decisions confirming the rule.
We can’t tell which is the insult and which is the injury — refusing to pay for the vast majority of services rendered, or slapping an inapplicable discount onto what remains. In total, AIG owes this QME $8,594.00, but has only paid $1,033.25. Without pursuing (and winning) the necessary appeals, the QME will lose $7,560.75.
Ignore California Fee Schedules & Increase Revenue
In California, every workers’ comp payer is incentivized to ignore the state fee schedules.
When the provider fails to dispute improper reimbursements by submitting Second Review appeals and paying $180 to file for IBR, the payer simply keeps the provider’s revenue. In California, when providers err the consequences are automatic. When payers err, providers must expend time, effort, and resources to chase their payment down.
It’s not personal, it’s just logic. It’s the law.
Fortunately, this provider is a client of DaisyCollect, our concierge billing service. On the provider’s behalf, DaisyCollect has already submitted a timely and compliant Second Review appeal for this travesty of an adjudication.
If necessary, we will appeal further — as should any physician in a similar situation.
Get paid in full and on time — without the hassle. DaisyBill makes authorization, billing, and appeals quicker, easier, better. Reach out to see how our software and services can help your practice.
CONTACT US
DaisyBill provides content as an insightful service to its readers and clients. It does not offer legal advice and cannot guarantee the accuracy or suitability of its content for a particular purpose.