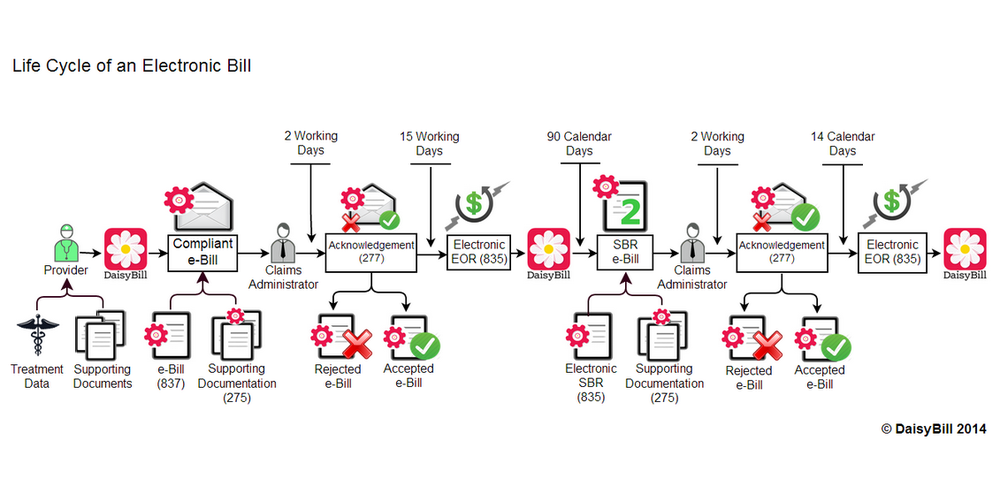
How Electronic Billing Works, Part I
If you’ve ever sent an email, you already have a general understanding of how workers’ compensation electronic billing works. So we’re going to use what you already know about e-mail to help you understand workers compensation electronic billing.
INSTANT SUBMISSION
With email, you write your message, click ‘send’ in your email client, and your message is sent instantly. You can’t make any changes or corrections, because your message is already on its way to the intended recipient.
Electronic Billing
In workers’ comp e billing, a bill submitter prepares the bill, clicks ‘submit’ in the computer software they’re using, and the electronic bill is instantly submitted. Just like an email, it can’t be changed or corrected because it’s already on its way to the claims administrator.
ACKNOWLEDGEMENT PROTOCOLS
Email Error Checking
Most emails make it to their intended recipient without any problems. However, if you've ever received an automated message from a mailer daemon, you know that some messages don't get sent as planned.
When you receive this automated message, you know that something went wrong with your send.
The automated messages help you solve the problem. Automated email responses explain what went wrong (red), utilize specific codes for errors (blue), and provide instructions for what needs to be done to resolve the issue (orange).
Electronic Billing Acknowledgement Protocols
In compliance with the California workers’ comp regulations for electronic billing, a claims administrator (or their EDI Agent) is in charge of setting up a system to check electronic bills for the following two errors:
- Incomplete electronic bill submissions.
- Electronic bill submissions where the injured worker is completely unidentifiable as the insured.
If either or these errors are detected, a claims administrator has 2 working days from submission to:
- Send the bill submitter codes that specifically describe the error (i.e. A6).
- Send the bill submitter codes that describe how to resolve the error (i.e. 629).
- Reject the electronic bill back to the bill submitter.
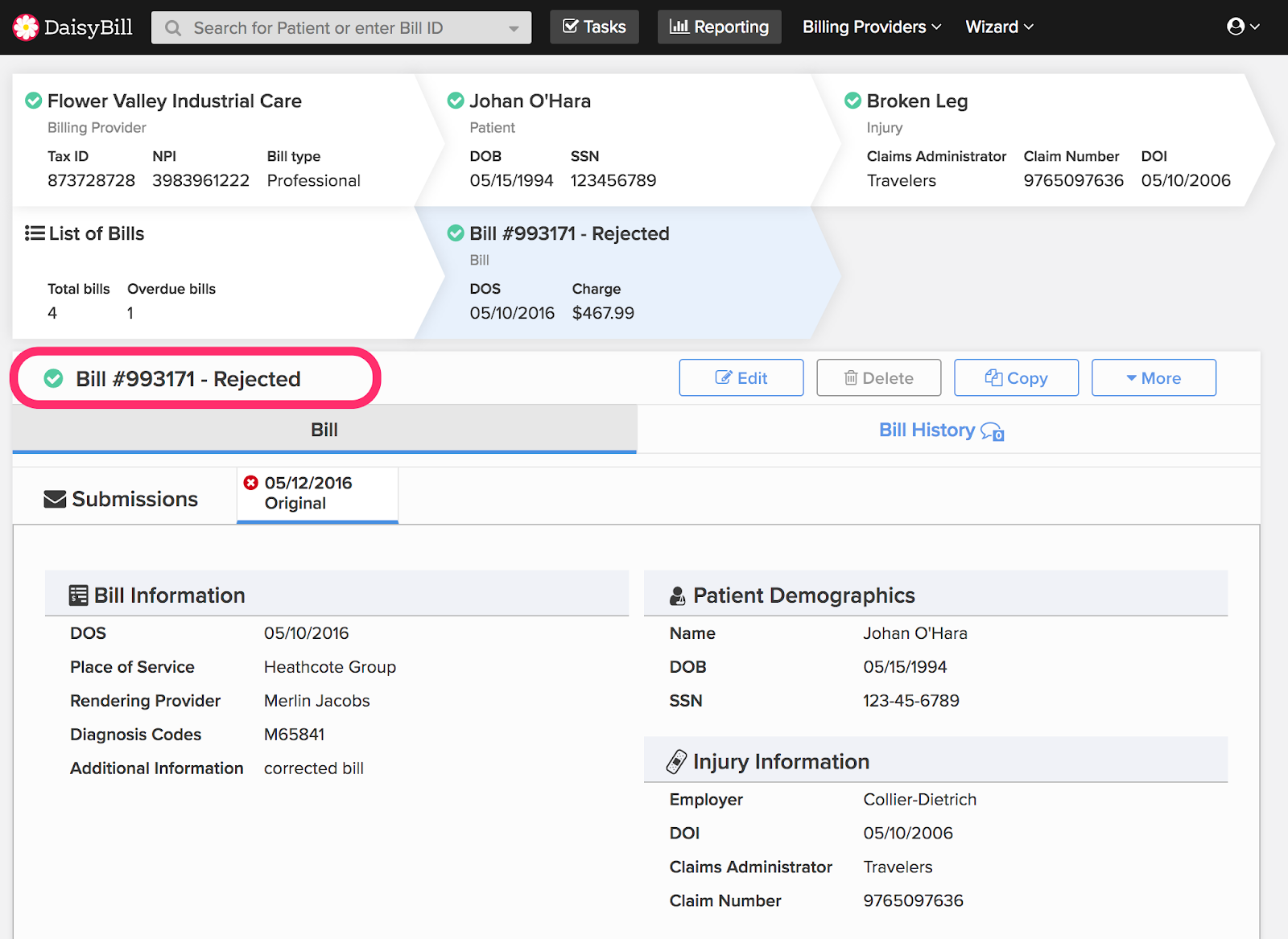
DaisyBill's system displays rejections as follows:
Just as emails rejected by a mailer daemon never make it to their intended recipient, electronic bills rejected by a claims administrator are never forwarded to the adjustor for review. As far as the intended adjustor is concerned, rejected electronic bills don’t exist.
The next post will cover what happens when electronic bills actually get to claims administrators.
DaisyBill provides content as an insightful service to its readers and clients. It does not offer legal advice and cannot guarantee the accuracy or suitability of its content for a particular purpose.