Doctors Beware: Do NOT Cash Three Rivers Network Check
A California doctor was recently surprised to find themselves subject to a 36-month discount reimbursement contract with terms that can only be described as sinister — and for no apparent benefit to the practice. Worse, it all happened because the doctor’s accounting department unknowingly cashed a mysterious check from Three Rivers Provider Network (TRPN).
Doctors Beware: Don’t let this happen to you.
Instruct accounting staff that depositing the TRPN check automatically ensnares the practice in an onerous agreement that:
- Allows TRPN to reduce reimbursements for workers’ comp, auto, and group health claims
- Allows TRPN to share the contractual discount with numerous entities
- Forbids a provider from extracting themselves from the contract for 3 years
The TRPN check comes with an attached document that appears to be — but is not — an Explanation of Review (EOR). If your office deposits the check, you must return the funds and inform TRPN that you do not wish to participate in their network within 90 days.
The details of TRPN’s…let’s say, unorthodox signature acquisition method are below. Be vigilant in avoiding this incredibly sneaky form of payment abuse.
Doctor Bills Zurich, Receives Reduced Reimbursement
This chilling story begins with an unexplained network discount applied to a bill the doctor sent to Zurich Insurance North America.
The doctor had made a concerted effort to cancel all Preferred Organization (PPO) and other network discounts draining the practice’s revenue (a wise decision, in our opinion). Therefore, the doctor was surprised to see a payment 5% below the amount the California Physician Fee Schedule allows.
In violation of California Labor Code Section 4609, the Zurich e-EOR did not name any specific discount reimbursement agreement or PPO. §4609 requires Zurich to “provide an explanation of benefits or explanation of review that identifies the name of the network with which the payor has an agreement that entitles them to pay a preferred rate for the services rendered.”
Since they had canceled all discount contracts, the doctor disputed the Zurich 5% reimbursement reduction by submitting a Second Review appeal, which stated:
This bill payment was incorrectly discounted citing a “PPO Discount.” This practice and provider do NOT have a PPO contract or agreement authorizing this payment discount. See supporting documents. Accordingly, please review this bill for additional payment per OMFS. Per Labor Code 4609 § (c)(2) the provider is requesting the entity demonstrate the entitlement to a reduced rate within 30 days. Failure to timely demonstrate that entity is entitled to the reduced contracted rate shall both: 1. Render entity responsible for the difference between the OMFS rate(s) and the reduced contract rate(s) used in paying the bill, which amount(s) shall be due and payable within ten (10) days of receipt of written notice, and 2. Bar entity from taking any future discounts without express written consent from provider.
TRPN “Reeducates” Doctor
TRPN sent an email to the doctor explaining that Zurich requested TRPN “reeducate” the doctor about the TRPN discount. The TRPN email included three attachments:
- A letter from the President of TRPN
- The information sent with the check the doctor unwittingly cashed
- The TRPN Contract
The letter attached to the email explained that the doctor had been under contract with TRPN since February of 2023, having “accepted our network participation payment” (i.e., depositing the $100 check) and subsequently failing to opt out of the contract within 90 days of depositing the payment.
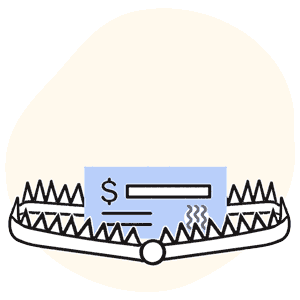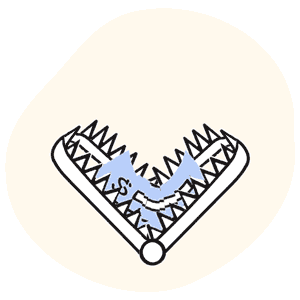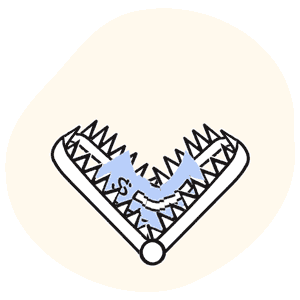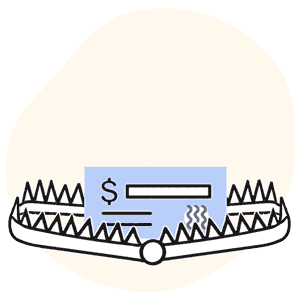
Unfortunately, the practice’s accounting department had cashed a check from the TRPN network. And unfortunately, the check was a Trojan horse — but instead of Greek soldiers, this horse was stuffed with some of the most rapacious network discount terms we’ve ever laid our horror-widened eyes on.
Important: with the check came a strange document formatted exactly like an EOR, but not for any sort of medical treatment reimbursement. Instead, where the details of payment denial or adjustment reasons would typically be found on an EOR, this TRPN document stated that the attached check was a “participation payment,” acceptance of which locked the provider into a network agreement.
The EOR-like document makes TRPN’s approach particularly eyebrow-raising. Many practices have separate accounting and/or billing departments, where an unwitting staff member may not look too closely at what (at first glance) appears to be a standard EOR and check.
As noted on the back, the check featured a “restricted endorsement” with an attached agreement. In other words, TRPN asserts that signing this check was legally equivalent to signing the TRPN agreement.
In a future article, we dig into the jaw-dropping details of the TRPN discount agreement. For now, when offered unsolicited payments from TRPN, every California doctor should take your parents' advice about the dangers of taking candy from strangers.
Workers’ comp billing requires specialized expertise. daisyCollect agents use our advanced software (and unmatched experience) to protect your practice’s bottom line. Request a demo below:
REQUEST DEMO
DaisyBill provides content as an insightful service to its readers and clients. It does not offer legal advice and cannot guarantee the accuracy or suitability of its content for a particular purpose.



.gif)



Absolutely disgusting.