Correct Electronic Bill Processing, Part II: Second Bill Review
A couple of weeks ago I posted a walk-through of correct workers’ comp electronic bill processing, starting from the original electronic bill submission to receipt of the electronic explanation of review (EOR). Today I’m posting a walk-through of correct processing for an electronic Second Bill Review (SBR), again using as an example the same actual electronic bill that we submitted to Sentry Insurance.
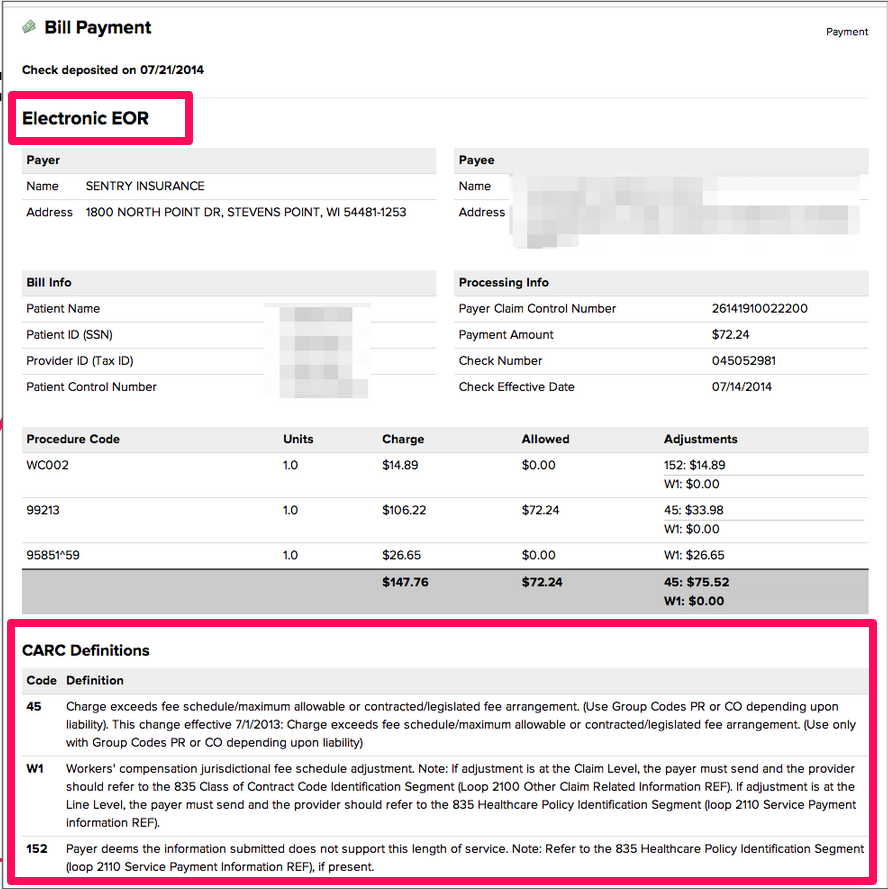
I’ll pick up where I left off--the electronic EOR for the original workers’ compensation electronic bill. Sentry correctly sent an electronic EOR in response to our electronic bill. Sentry also did a great job of following the rules by setting out the reasons for adjustments so that the provider could determine whether or not an SBR should be filed.*
This bill history shows that the provider decided to submit an SBR and submitted it on July 21st along with the required supporting documentation. Like the original electronic bill, the electronic SBR must go through Sentry’s clearinghouse, Stoneriver P2P.
Remember that if you submit an original bill electronically then any SBR must be electronic as well. As in the case of the original electronic bill, daisyBill calculates when the Final EOR is due, which for this SBR is August 4th, in 14 calendar days.
The history then shows Sentry’s clearinghouse, StoneRiver P2P, accepting the SBR the next day.
10 days after daisyBill submitted the SBR, Sentry sent back an electronic Final EOR on 7/31 which is 4 calendar days prior to the DWC-mandated deadline.
Three important points I would like to note:
1. Sentry followed the rules for electronic billing to the letter, including adhering to timelines, returning electronic EORs, and setting out clear and compliant reasons for adjustment. We’d like to recognize Sentry for being a good citizen in the workers’ comp community.
2. Notice that Sentry remitted an additional $10.12 which, if we were dealing with submitting a paper SBR, would barely be worth the staff time and printing and mailing costs. However, electronic SBRs are incredibly easy and take literally seconds to submit. Because all the provider, patient, and injury information is already in the electronic billing system, that information can be pre-populated in the online SBR form. The only field that providers need to fill out is the reason for submitting an SBR-- and the electronic Final EOR should tell you exactly what needs to be in that field.
3. Even if you’re not electronic billing, providers should file an SBR for every single under-payment, no matter how low the amount. This isn’t just for the benefit of the bottom line (all those small amounts add up), but also to encourage proper claims processing. And, back when I was billing for a medical practice, I found out that appealing every underpayment paid off in the long run because claims administrators learned that I was too much of a pain in the b*** to pay incorrectly. Hah!
*If a provider disputes the amount of payment, the provider must send the claims administrator a compliant SBR with details describing the reason for disputing the payment. The provider must send the SBR within 90 days of receipt of the EOR.
DaisyBill provides content as an insightful service to its readers and clients. It does not offer legal advice and cannot guarantee the accuracy or suitability of its content for a particular purpose.