🔎 Search Thousands of IBR and IMR Decisions 🔎
With two new workers’ comp tools, searching through past decisions just got a whole lot easier:
- DWC’s announces super-useful search tool for Independent Medical Review (IMR) decisions.
- daisyBill releases new (and pretty spectacular) search tool for Independent Bill Review (IBR) decisions.
1. DWC Search Tool for Workers’ Compensation Independent Medical Review (IMR)
IMR Refresher:
Before rendering service, a provider must file a Request for Authorization. If utilization review denies, delays, or modifies a treating physician's request for medical treatment, the injured worker can request a review of that decision by filing a request for Independent Medical Review (IMR).
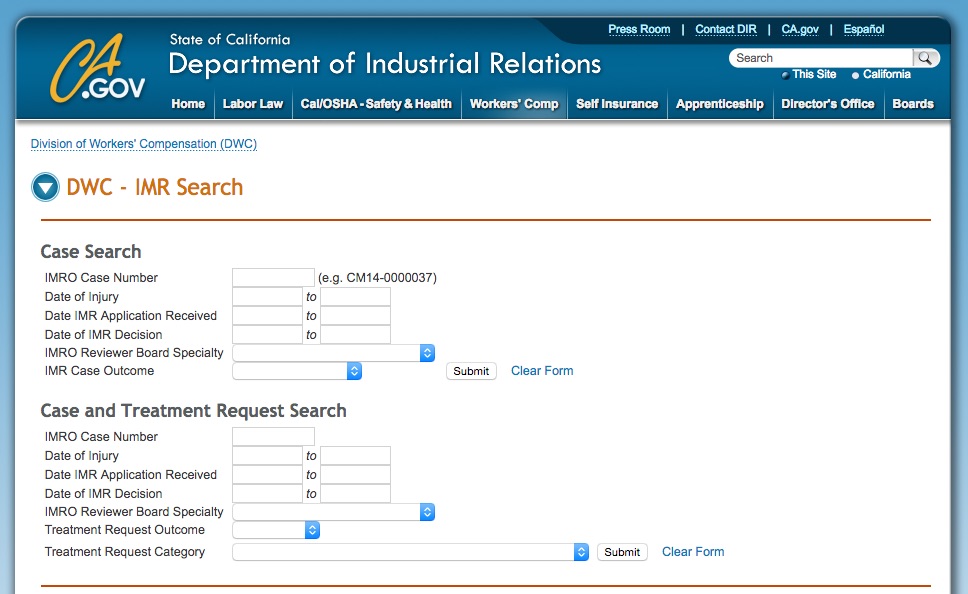
On May 12th, 2016, the DWC issued DIR Newsline 2016-51 announcing a new search tool for workers’ comp IMR decisions.
Since the implementation of the IMR process on January 1st, 2013, injured workers filed 300,000+ IMR cases. Previously, the DWC posted the decisions, but it was not possible to sort and search the decisions.
But thanks to the DWC’s nifty new IMR Search, users can now go to the DWC website and search the IMR database, applying filters such as:
- case number,
- date of injury,
- specialty of reviewer,
- and/or category of treatment request.
We couldn’t agree more with David DePaolo’s praise of the DWC, and his opinion that the new IMR search tool “should lead to much better oversight and administration of the IMR process, in addition to providing parties with much needed confidence that the system is, or isn't as the case may be, working properly.”
2. daisyBill’s Independent Bill Review (IBR) Decision Search
IBR Refresher:
In contrast to IMR, which occurs before treatment, Independent Bill Review (IBR) occurs after treatment, when a provider disputes a bill payment. While an injured worker submits an IMR, a provider submits an IBR. The DWC’s IBR page explains the specific requirements for filing an IBR.
Like IMR decisions, the DWC posts all IBR decisions on the DWC website; but unlike IMR decisions, the DWC hasn’t yet released a search tool for them.
daisyBill to the rescue!
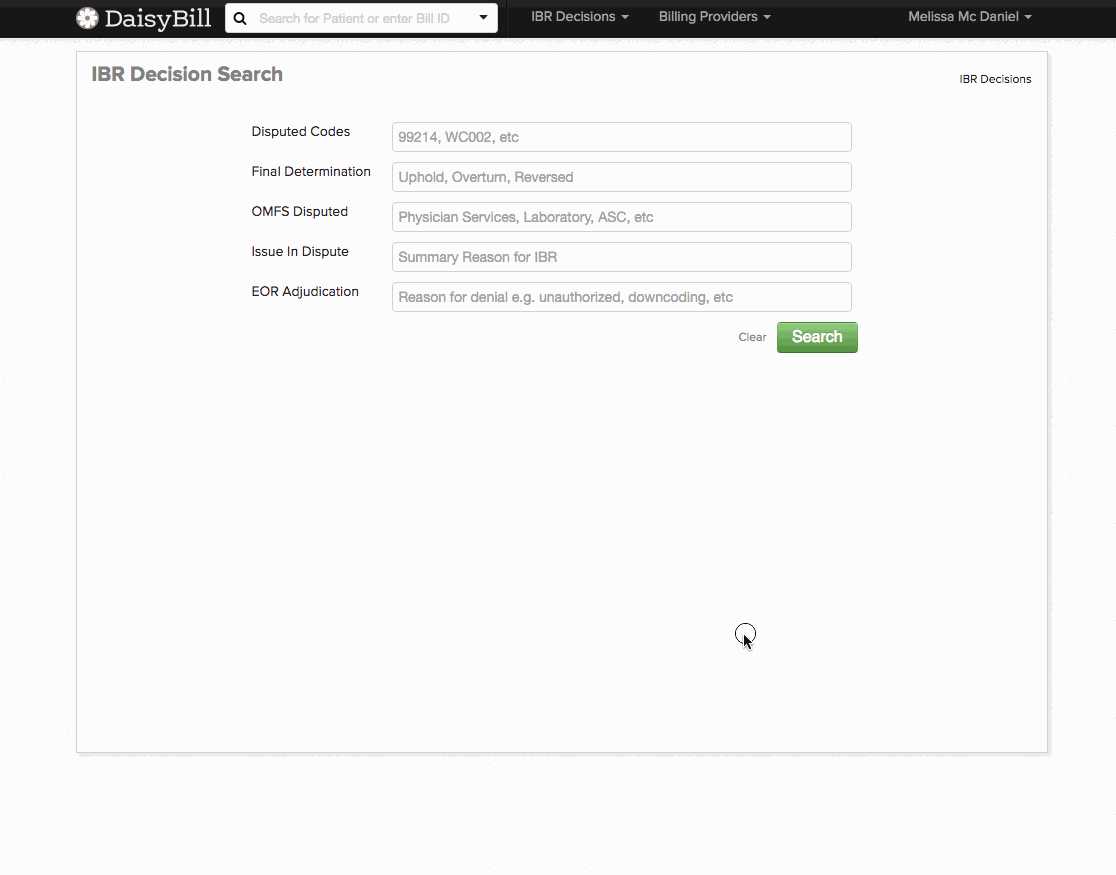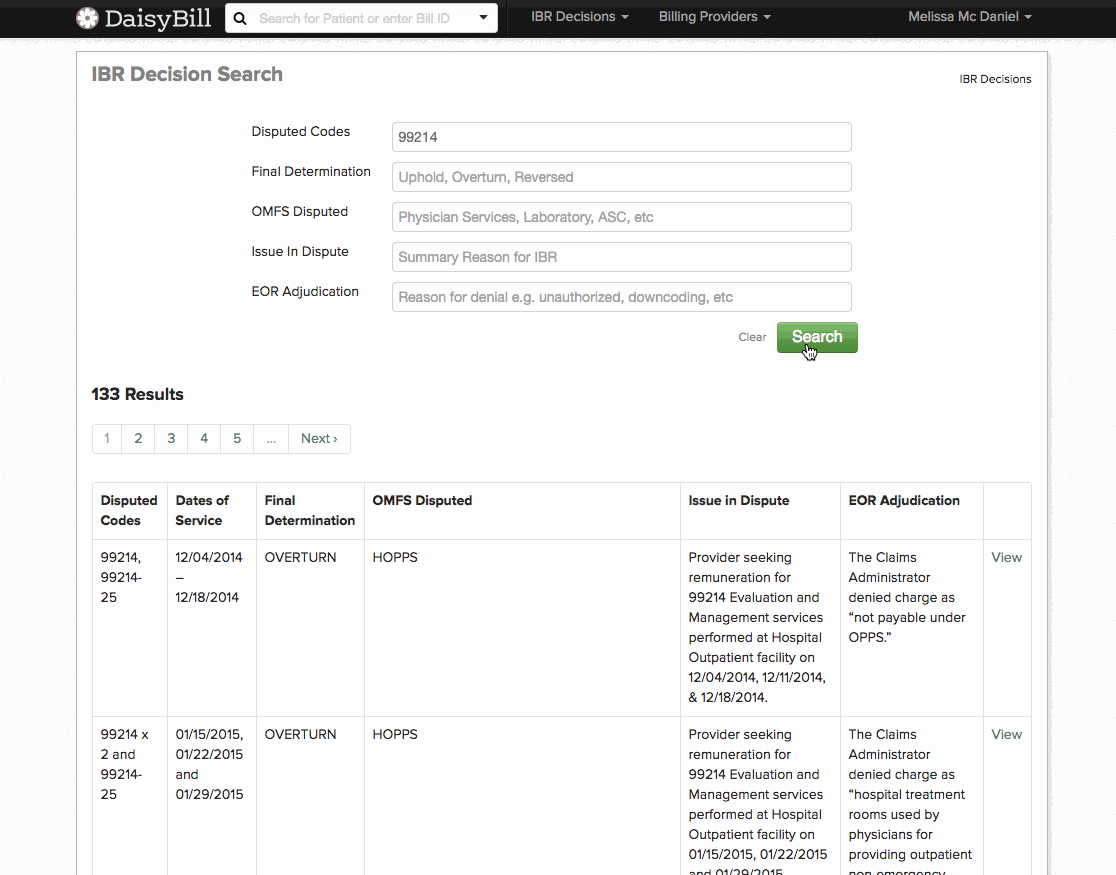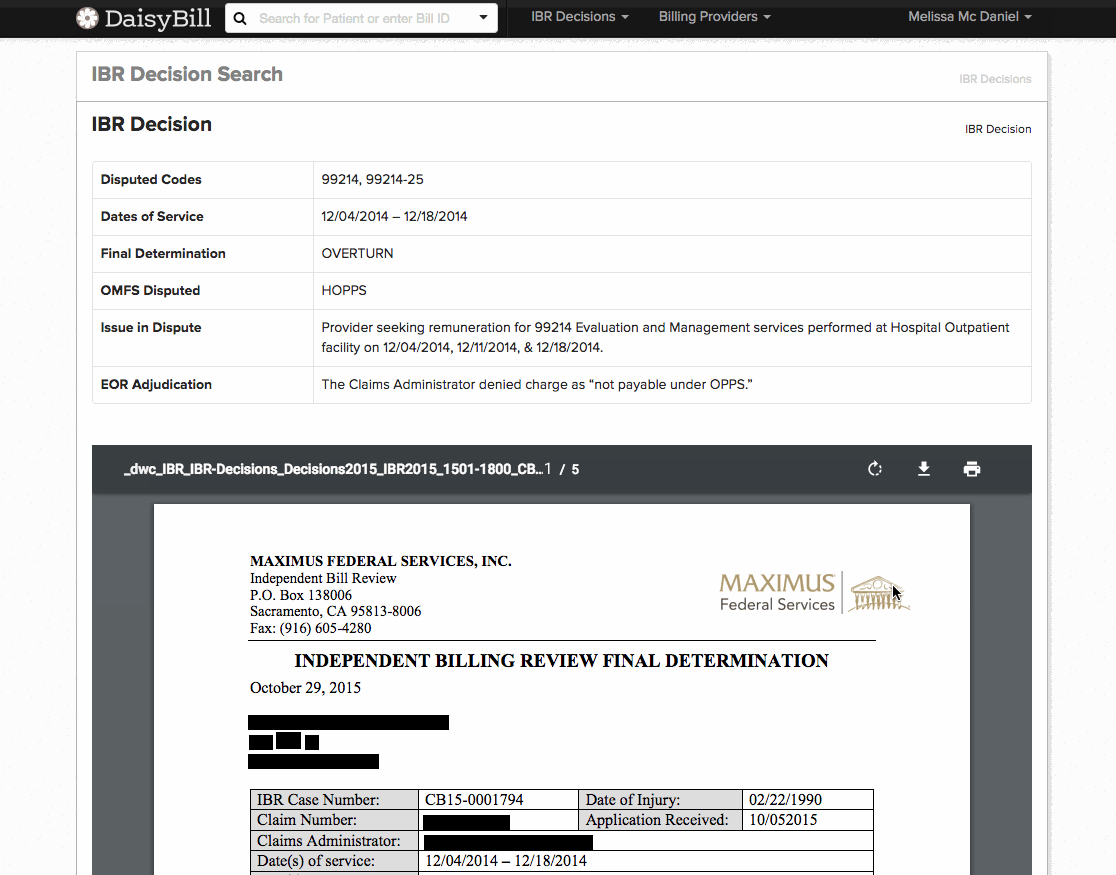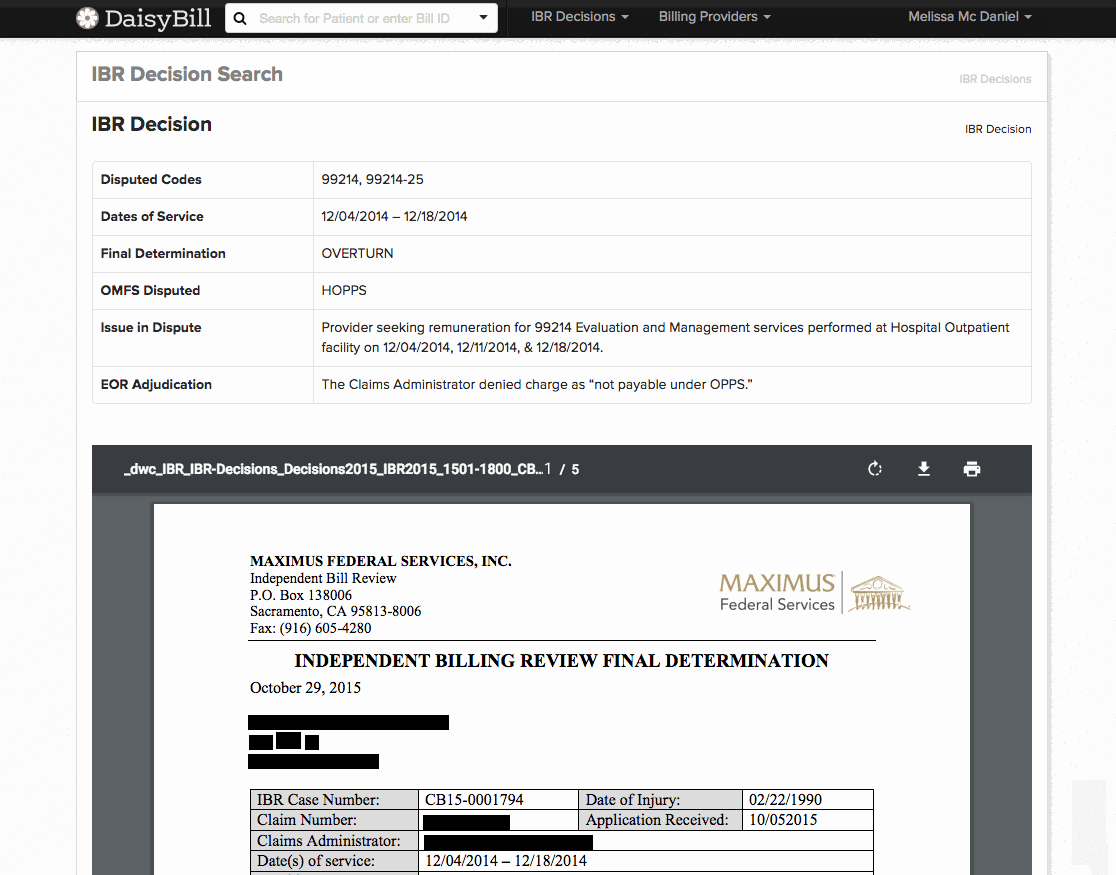
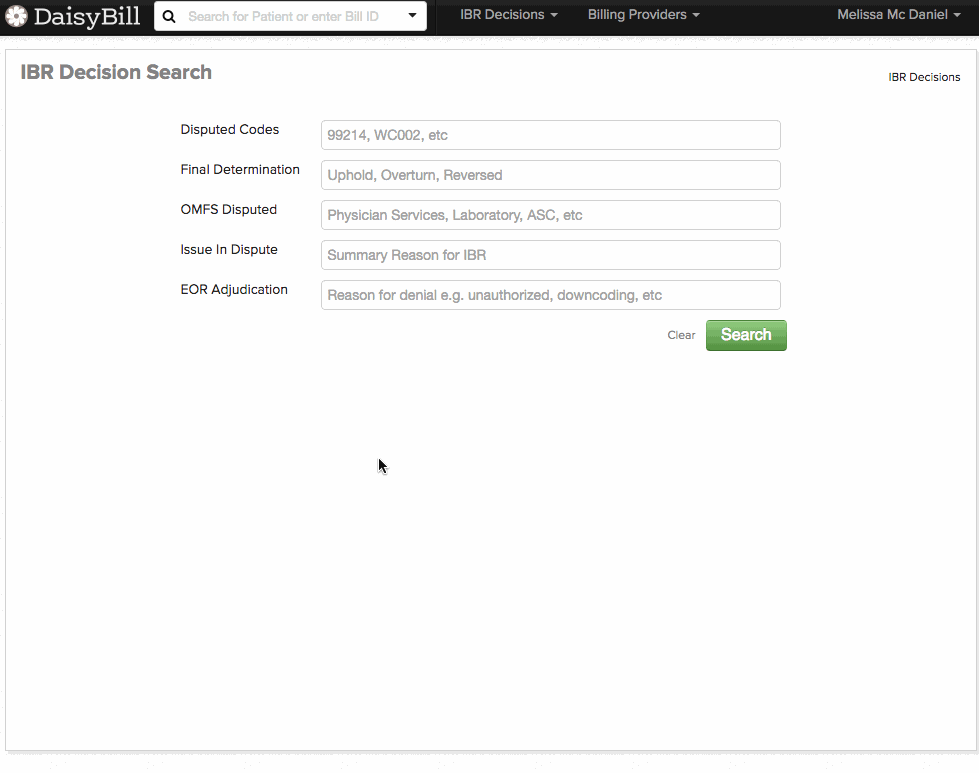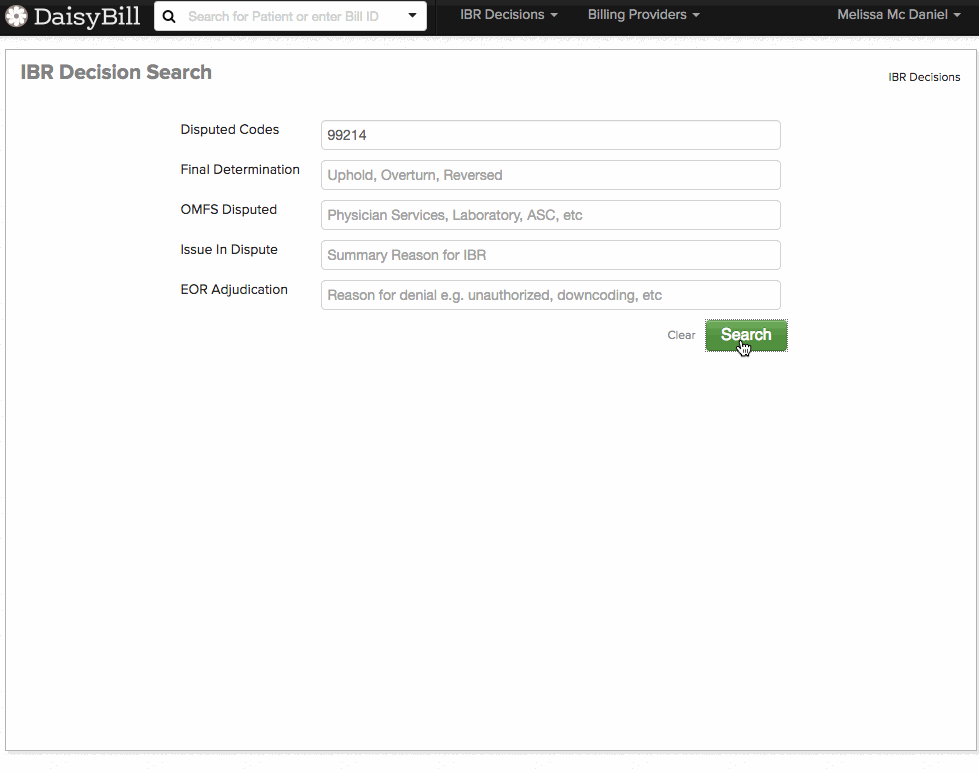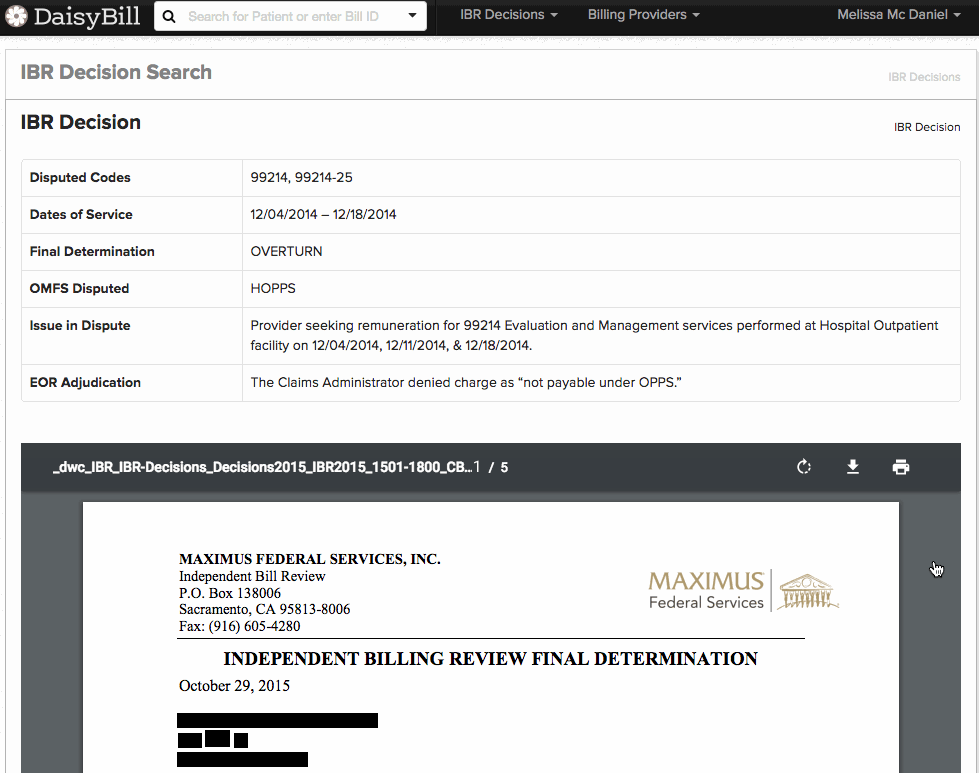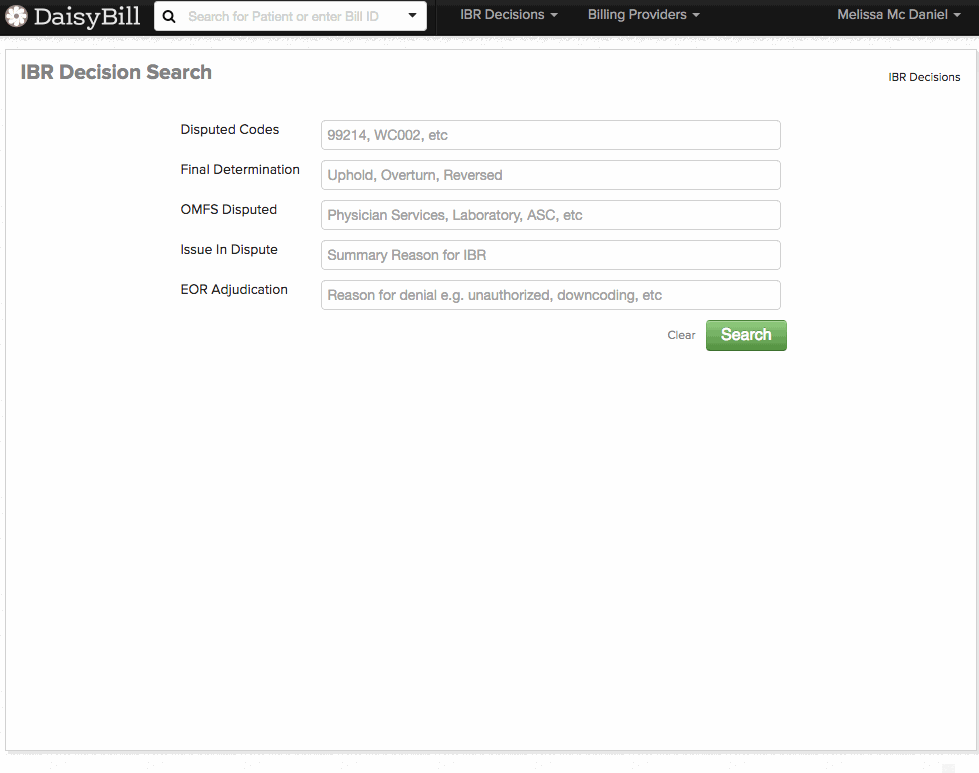
For fast, convenient IBR look-up, daisyBill created our user-friendly IBR Decision Search. daisyBillers can now access and filter over 4,000 IBR cases, which is a fantastic resource for finding the exact IBR decision that addresses your issue. We developed this search specifically with Second Reviews in mind, because a relevant IBR decision is powerful support for a request (or denial) for additional payment.
To use the new search tool, simply type in and search for:
- A disputed billing code (such as 99214)
- Final determination (upheld, overturned, or reversed)
- Fee schedule disputed (Physician Services, Laboratory, etc.)
- Issue in dispute (such as consultation reports)
- EOR Adjudication (unauthorized, not payable, downcoding, etc.)
For non-daisyBillers, get instant access to our IBR Decision Search with a free 3-day trial.
Upcoming Webinar: Second Review Strategy Kit
Before the IBR stage, providers and claims administrators must first go through the Second Review process. Watch our webinar, Second Review Strategy Kit.
In this free webinar we cover the specifics that make all the difference between payment and another denial.
WATCH WEBINAR
DaisyBill provides content as an insightful service to its readers and clients. It does not offer legal advice and cannot guarantee the accuracy or suitability of its content for a particular purpose.
.gif)

