Second Bill Reviews for Work Comp: Claims Admin Mistakes
A few days ago I posted examples of good and bad SBR EORs returned by claims administrators. Today I’m posting another SBR denial which shows two mistakes that claims admins make when processing work comp SBRs.
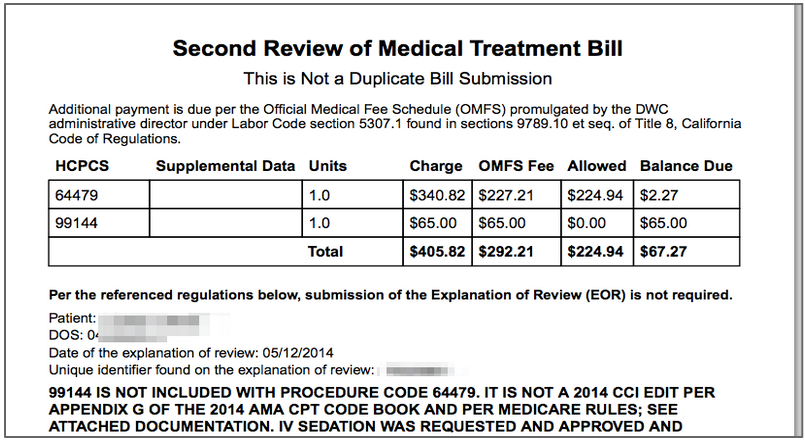
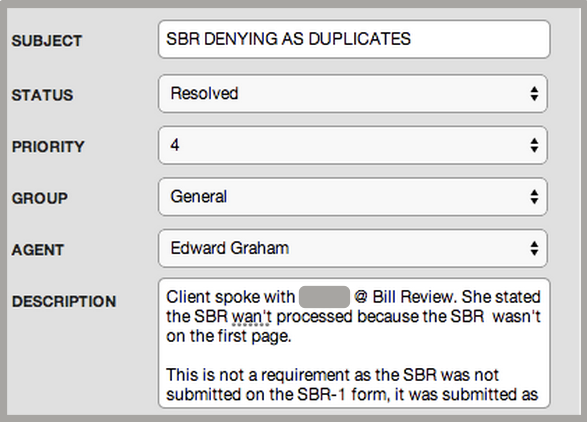
DaisyBill sent a complete and compliant SBR to PG&E, a section of the first page of which I’ve pasted below. Note that we sent the SBR as a modified original bill and not on an SBR-1 Form. The DWC does not require the SBR-1 form and will accept a properly modified original bill. PG&E denied the SBR on the grounds that it was a duplicate submission, but the section below clearly states that it is an SBR and that is not a duplicate bill submission.
So what happened? When contacted, it turns out that PG&E had made two mistakes when processing the SBR.
The first mistake was the same type of mistake that AIG made in the example from a couple of days ago--incorrect denial code. PG&E’s denial actually had nothing to do with the SBR being a duplicate bill submission. I don’t know why claims administrators sometimes use incorrect denial codes for work comp bills but it just slows down the whole process.
Anyway, PG&E’s actual reason for denial--and its second mistake--was that we did not use the SBR-1 Form as the first page of the submission. However, when providers don’t use the SBR-1 Form then, as should be obvious, the SBR-1 Form does not need to be the first page of the SBR submission. In fact, in such a circumstance, the SBR-1 Form doesn’t need to be part of the SBR at all.
Another thing I want to point out is that it may seem not worth the trouble to file an SBR for $67.27, as in the example above. But I always urge our providers to seek payment of every cent owed--its very easy with DaisyBill and the rewards are worth it. Even when it seems like it would be a pyrrhic victory because of the low additional reimbursement, it’s not the individual amounts that matter so much as sending a message that your practice is too much of a pain in the butt to pay incorrectly. The bigger picture, of course, is that prodding correct reimbursement behavior contributes to a better functioning workers’ compensation system for all of us.
DaisyBill provides content as an insightful service to its readers and clients. It does not offer legal advice and cannot guarantee the accuracy or suitability of its content for a particular purpose.