New York: Changes to Workers' Comp DME Authorization
Attention New York medical providers: the Workers’ Compensation Board (WCB) changed how it handles some requests for Durable Medical Equipment (DME) for injured workers.
According to a recent WCB bulletin, the change applies to cases where:
• The provider submits a Prior Authorization Request (PAR) for a DME item, and
• The Official New York Workers’ Compensation DME Fee Schedule does not list a price for the DME item, and
• The WCB issues an Order of the Chair (OOC) to resolve the PAR
In such cases, OOC will note the provider’s cost estimate for the DME item in question. Additionally, on March 27, the WCB deleted all draft PARs and draft payer responses to PARs in the OnBoard system, through which providers submit all PARs.
Providers may have to re-initiate all draft PARs they did not submit before 6 PM Eastern on March 27, 2025.
NY Workers’ Comp PARs
In New York workers’ comp, providers generally do not have to submit a PAR when the state’s Medical Treatment Guidelines (MTGs) recommend the treatment in question.
While providers have the option of submitting PARs to confirm MTG compliance, PARs are only a requirement for:
- Treatments that the MTGs do not list
- Variances from the MTG
- Non-formulary medications
- “Special Services” as defined in the MTGs
- DME that is not in the Official DME Fee Schedule or that the DME Fee Schedule specifically lists as requiring a PAR
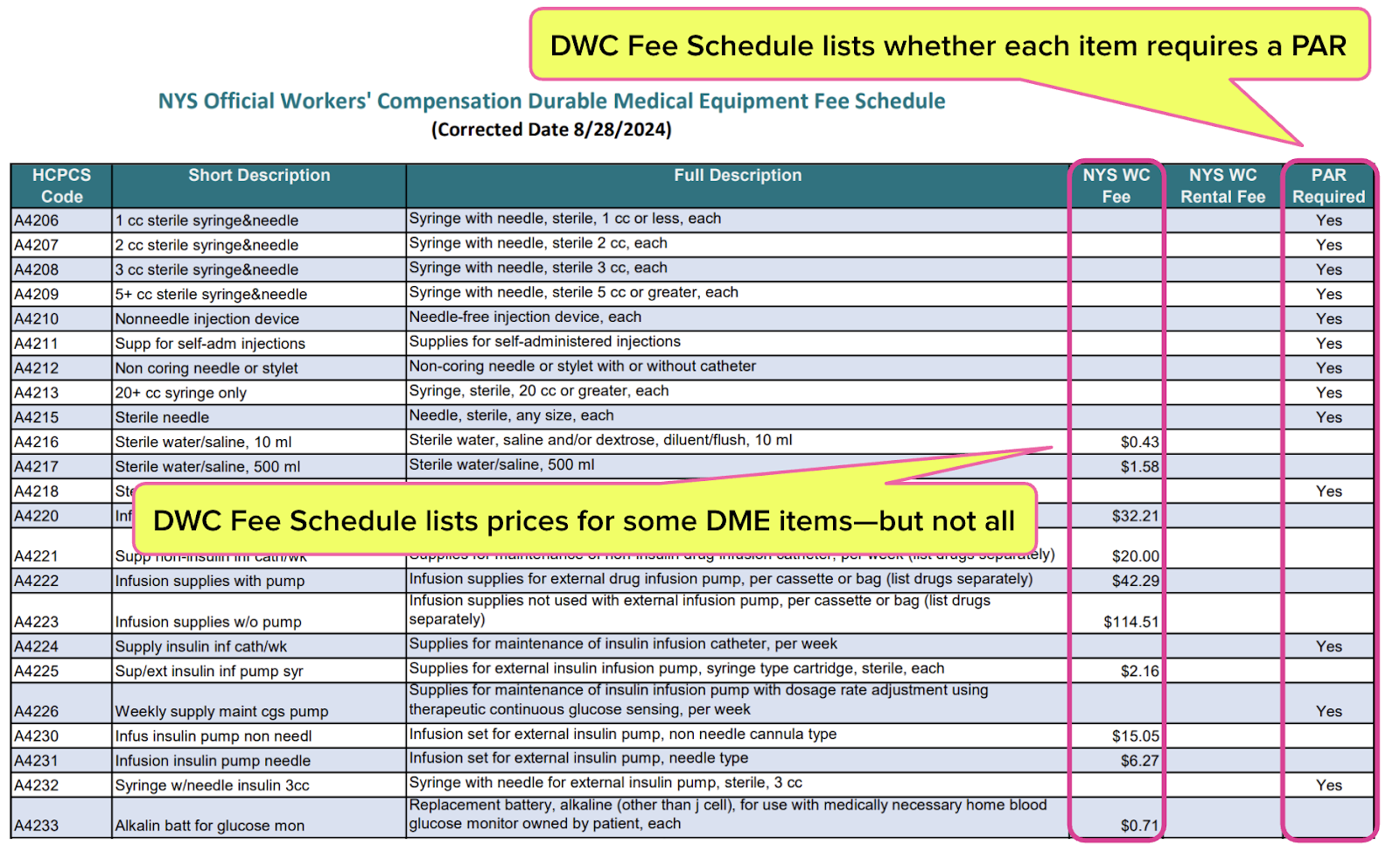
The DME Fee Schedule (screenshot below) indicates whether the provider must submit a PAR for each DME item and the “NYS WC Fee” for the item where applicable.
New Enhancement: DME Not in Fee Schedule
The screenshot above shows that the DME Fee Schedule does not list a “NYS WC Fee” for some DME items. According to an OnBoard News release, in cases where the provider submits a PAR for DME, and the DME Fee Schedule does not list the price (emphasis ours):
“...the estimated cost provided by the provider for the DME item in a PAR will be noted on all subsequently issued Orders of the Chair [OOC].”
According to the WCB’s PAR Process page, when a provider uses the OnBoard system to submit a PAR, OnBoard automatically tracks the deadline for a claims administrator to respond to the PAR. For DME, the deadline to respond to a PAR is four calendar days.*
If the claims administrator fails to respond to a PAR timely, the WCB may issue an OOC.
WCB Deleted Draft PARs March 27, 2025
According to the OnBoard News release, the WCB deleted all draft PARs from providers and provider delegates (along with all draft PAR responses from payer reviewers) in the OnBoard system at 6 PM on March 27.
Providers may wish to confirm if there were any draft PARs in the system that they or their delegates did not submit before the mass deletion. If so, be sure to re-initiate the process of submitting these PARs.
daisyBill experts are eager to help New York providers comply with WCB requirements, especially as the August 2025 deadline for mandatory workers’ comp electronic billing approaches. Use the pink chat icon in the bottom right of this screen, or reach us at info@daisybill.com. We’re here for you!
*Subject to the state’s General Construction Law regarding weekends and holidays
Mandatory e-billing for NY workers’ comp starts August 1, 2025. daisyBill makes it easy, with payment in less than 10 days on average. Schedule a call to learn more.
SCHEDULE CALL
DaisyBill provides content as an insightful service to its readers and clients. It does not offer legal advice and cannot guarantee the accuracy or suitability of its content for a particular purpose.


.gif)



