City and County of San Francisco's Misleading Response in PPO Discount Dispute

Recently, a DaisyBill provider disputed a reduction in reimbursement from the City and County of San Francisco (CCSF) for treating an injured employee. In the Explanation of Review (EOR) CCSF sent to the provider, CCSF justified taking 10% from the reimbursement by citing a First Health PPO contract.
CCSF’s reasoning has one glaring issue: According to Coventry/First Health, they cannot locate a contract between this provider and First Health.
Worse, CCSF assured California’s Division of Workers’ Compensation (DWC) that the provider signed the contract in question. Despite CCSF providing no documentation or other proof of this nonexistent agreement, the DWC took CCSF at its word.
The Dangers of PPO Discounts
We have written extensively about how payers use Preferred Provider Organization (PPO) contracts to hustle workers’ compensation providers out of complete reimbursement. Payers simply apply a PPO contract name to the EOR and reduce the reimbursements to below those dictated by the state’s Official Medical Fee Schedule (OMFS).
In some cases, these PPO contracts force providers to accept an up to 30% reduction below OMFS reimbursement rates. Providers typically sign PPO contracts because they believe the PPO will direct more patients to the practice. However, PPOs do not direct patients to providers.
Once a provider signs a PPO discount contract, the discounts can be leased, sold and transferred to many different payers. Each of these payers can take money from a provider by simply citing the PPO contract name on the EOR. The payer and/or PPO keeps provider revenue, while providing zero treatment or services to injured workers.
Below, we walk through this provider’s ordeal, and take a close look at CCSF and its vendors’ arguably misleading representations in response to the dispute. This tale exposes the impunity with which claims administrators like CCSF use unverifiable PPO contracts to take advantage of providers and subvert California workers’ comp.
Provider Submits Second Review Appeal
January 15 2021: The provider submitted a Second Review appeal to dispute the PPO reduction CCSF took. The EOR that CCSF sent the provider listed “First Health” as the PPO contract that allows CCSF to take a cut of the provider’s revenue.
In the Second Review appeal, the provider asserted that the provider does not have a PPO contract with First Health:
"The EOR identifies First Health as the entity that entitles City and County of San Francisco (CA) to pay a preferred rate for the services rendered. The Provider asserts that the reduced rate is incorrect because no contract or agreement exists between First Health and [the provider] that allows City and County of San Francisco (CA) to pay a preferred reduced contracted rate to the Provider."
In the appeal, the provider invokes California Labor Code Section 4609 (c)(2), challenging CCSF to demonstrate its right to discount the provider's reimbursement.
"Per LAB 4609 § (c)(2), [the provider] has the right to request that City and County of San Francisco (CA) demonstrate its entitlement to pay [the provider] a reduced contracted rate. Once requested, the claims administrator must make this demonstration within 30 business days of receipt of the request. This letter serves as such a request.”
In responding to the Second Review appeal, CCSF ignored the provider’s request for documentation of its supposed discount rights. Rather than providing the requested First Health contract, CCSF simply denied the appeal, and continued to withhold full OMFS reimbursement.
Provider Requests Independent Bill Review
February 5, 2021: Following CCSF’s Second Review denial, the provider paid $180 to file a request for Independent Bill Review (IBR) with Maximus, the state-appointed arbiter of workers’ comp payment disputes. Per IBR protocol, Maximus offered CCSF a formal opportunity to dispute the case’s eligibility for IBR “by submitting a statement with supporting documentation.”
February 19, 2021: EK Health — apparently a sidekick CCSF vendor — replied to Maximus on behalf of CCSF. EK Health told Maximus that the provider has maintained a contract with “Coventry/First Health” since 2004, and that Coventry/First Health will not share the contract with Maximus. With no other explanation, EK Health states that the network is “unable to share contract language as this can only be shared with the provider.”
EK Health’s full response is reproduced below:
Despite having addressed this kind of contract dispute on multiple previous occasions, Maximus chose to refer the case back to the DWC.
DWC Rules IBR Ineligible Despite Precedent (and DWC FAQs)
March 8, 2021: The Administrative Director of the DWC (“AD”) sent the provider a letter stating that the dispute is ineligible for IBR. Specifically, the letter from the AD states “Here, the payment dispute involves the applicability of a PPO contract to the provider. This is not an issue that can be resolved through the independent bill review process.”
This decision by the DWC directly contradicts dozens of past decisions by Maximus on the exact same contract dispute issues.
For example, in the Maximus IBR final determination for Case # CB19-0001503:
"EORs reflect a PPO discount of 20%, Provider is disputing the PPO discount stating that there is no Contract with the PPO Network reflected on the EOR. The Assignment letter with a request for a copy of the Contract to support the PPO discount for DOS 08/05/2019 was issued to the Claims Administrator on 12/20/2019. Response not yet received. 72141 Overturned.”
Furthermore, DWC FAQs clearly state that IBR is appropriate for disputes associated with contract reimbursements. From the DWC’s IBR FAQ page:
"If the medical service is covered by a fee schedule adopted by the Division of Workers’ Compensation (DWC), for example treatment under the Physician Fee Schedule or an evaluation under the Medical-Legal Fee Schedule, or set forth in a contract for reimbursement (Labor Code section 5307.11), then SBR and IBR must be utilized to resolve the dispute within a matter of weeks, as opposed to possible years under the WCAB lien system."
Coventry Admits: Contract Cannot Be Located
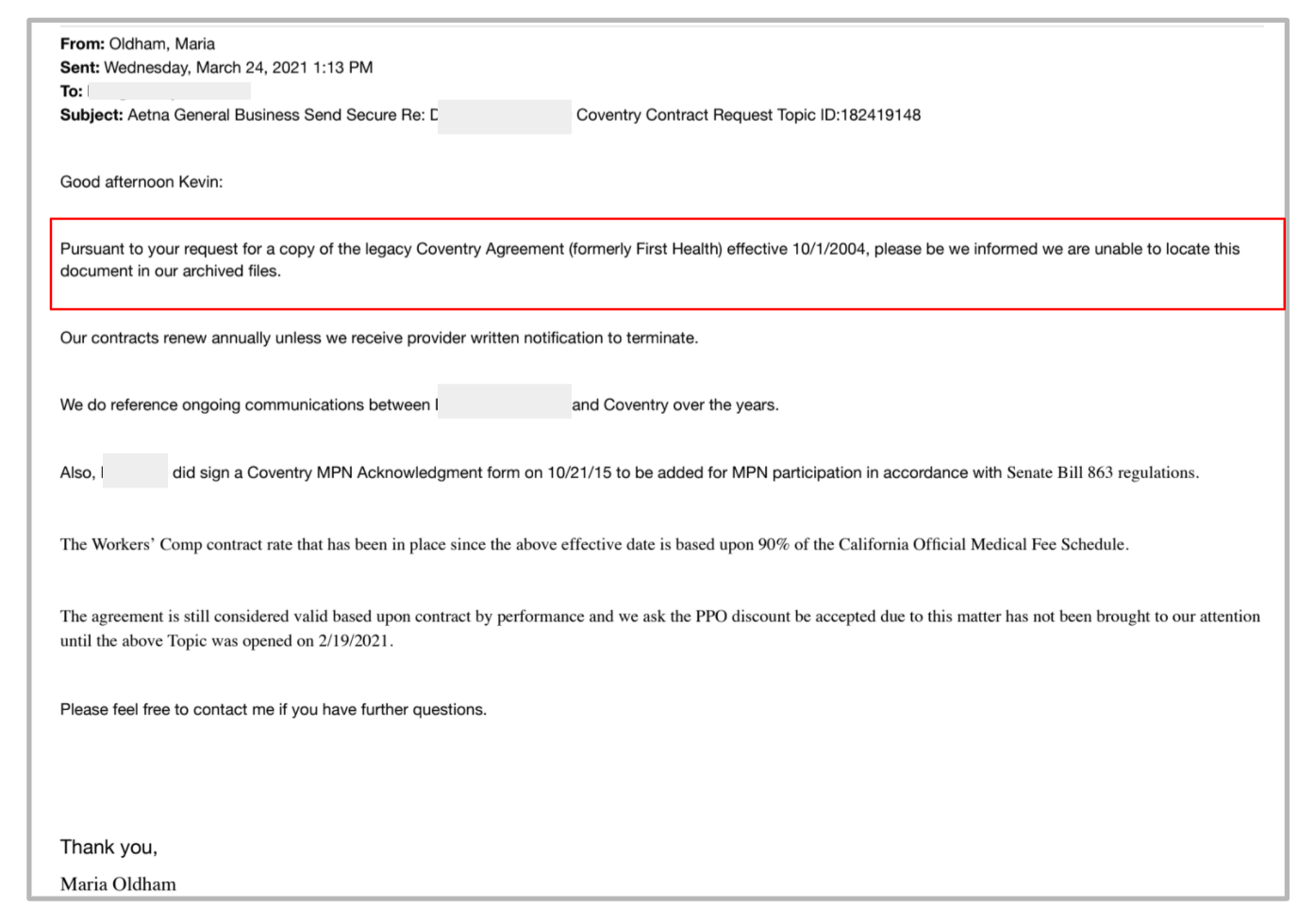
March 24, 2021: In reference to a separate dispute regarding the same (supposed) contract, Coventry emailed the provider, admitting they cannot locate the contract in question. In the email, a Coventry representative acknowledged:
Pursuant to your request for a copy of the legacy Coventry Agreement (formerly First Health) effective 10/1/2004, please be we informed we are unable to locate this document in our archived files.
The email confirms one very salient point: when EK Health claimed that Coventry/First Health could not share the contract with Maximus for the purposes of IBR, they were — in strictly professional terms — full of it. While EK Health’s letter claims the contract “can only be shared with the provider,” the fact is that CCSF, EK Health, and Coventry/First Health had no contract to share.
With anyone.
This raises two serious questions:
- What does the missing contract mean with regard to CCSF’s representation to Maximus (via EK Health) that the network was “unable to share contract language as this can only be shared with the provider”?
- Why did the DWC accept the arguably specious excuse that the network was “unable to share contract language as this can only be shared with the provider”?
In the email below, instead of producing a valid contract, Coventry tries to indicate that the provider implicitly agreed to allow Coventry to take 10% of the provider’s revenue because the provider agreed to be in the MPN.
Even more alarming, Coventry’s email suggests the provider should continue to accept the discount "due to this matter has not been brought to our attention until the above topic was opened on 2/19/21.” This perversion of the English language is rivaled only by its perversion of logic. The provider should continue to accept reductions in exchange for what, exactly?
Despite the DWC’s clear error in declaring this dispute ineligible for IBR, the facts remain. CCSF, et al claimed an unearned PPO discount from a provider, and cannot substantiate their right to do so. We sincerely hope that DaisyBill is not the only party willing to take a closer look.
When claims administrators misbehave, DaisyBill has your back. Enjoy fast, accurate payment, easy appeals and more with our Billing Software. Contact us to learn more.
CONTACT DAISYBILL
DaisyBill provides content as an insightful service to its readers and clients. It does not offer legal advice and cannot guarantee the accuracy or suitability of its content for a particular purpose.