Gallagher Bassett Flips UR Decision, Confusion Reigns

To an injured worker denied the care their treating physician deems necessary, California’s Utilization Review (UR) process can seem arbitrary, even cruel.
This perception is not helped when claims administrators like Gallagher Bassett reverse UR decisions with no material change in the facts, making those decisions appear like random determinations of medical necessity or lack thereof.
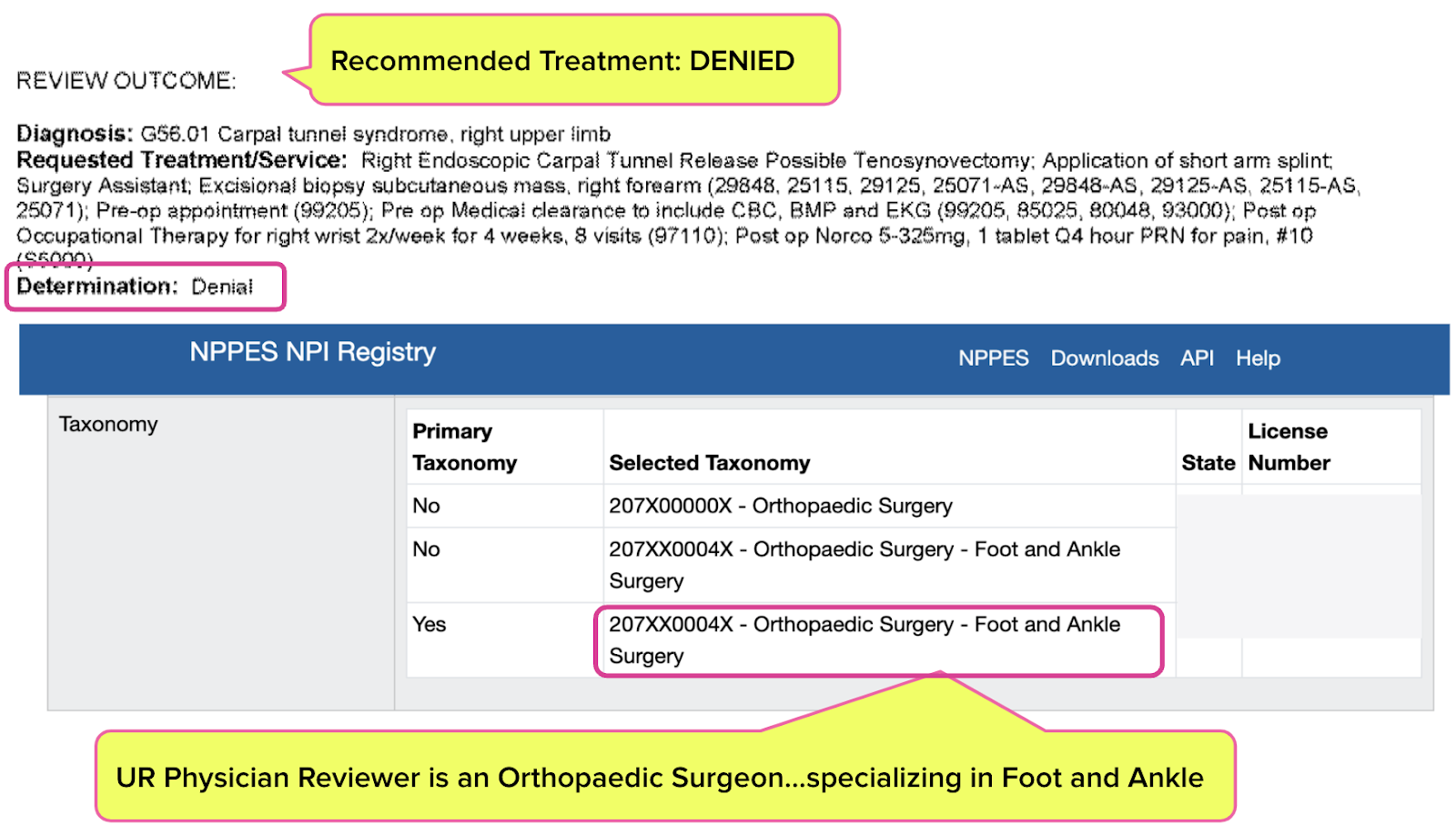
A Gallagher Bassett UR physician (a foot and ankle orthopedist) denied carpal tunnel surgery for an injured worker. When the injured worker’s physician resubmitted the exact same Request for Authorization (RFA), with the exact same medical documentation, Gallagher Bassett did a 180°, approving surgery.
We’re happy the injured worker will receive the treatment recommended by their doctor. But decisions and reversals like this make UR look less like an objective medical necessity assessment and more like a coin toss.
Gallagher Bassett Nixes Surgery
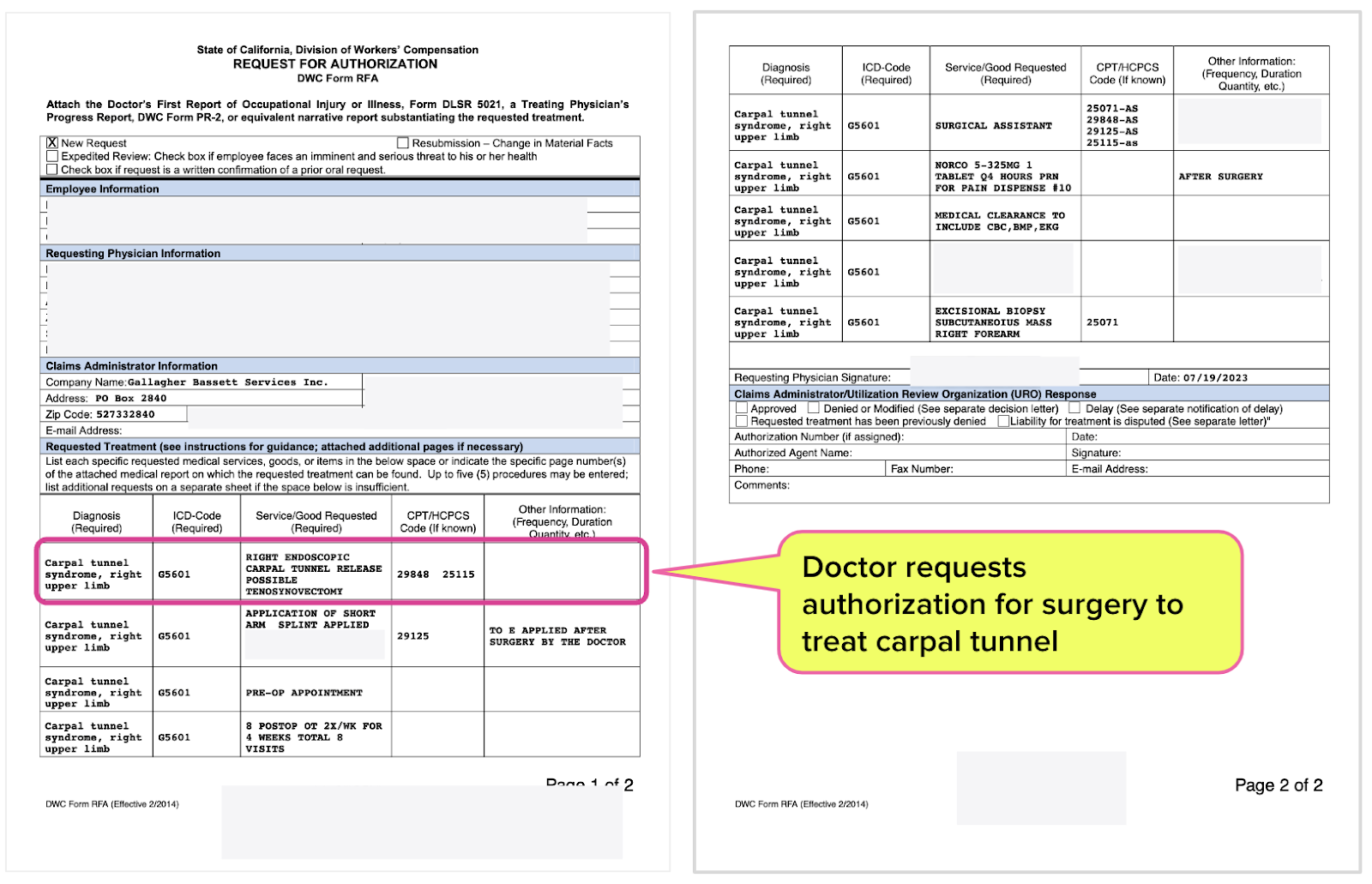
When more conservative treatments failed, the treating physician determined that surgery was the only way forward for a worker beset by carpal tunnel syndrome.
The physician submitted an RFA to Gallagher Bassett, complete with extensive documentation of diagnostic tests, including radiographs, MRIs, and ultrasounds.
Per the treating physician, the injured worker “has clinical and ultrasound evidence of carpal tunnel syndrome. [They] had a nerve conduction study in the past that indicated carpal tunnel syndrome.”
But GB Care, Gallagher Bassett’s UR organization (URO), denied the recommended surgery for the right upper limb (i.e. the hand/wrist).
Of note, the UR physician denying the surgery was a foot and ankle orthopedic surgeon.
Gallagher Bassett Flips UR Decision
Following the denial of surgery, the injured worker’s treating physician sent Gallagher Bassett a second RFA requesting the surgery (again).
RFA #2 included precisely the same supporting medical documentation as RFA #1. We know the documentation submitted with RFA #1 and RFA #2 are the same, because daisyAuth maintains a record of every RFA and document faxed through our system. Comparing the two submissions was all too easy.
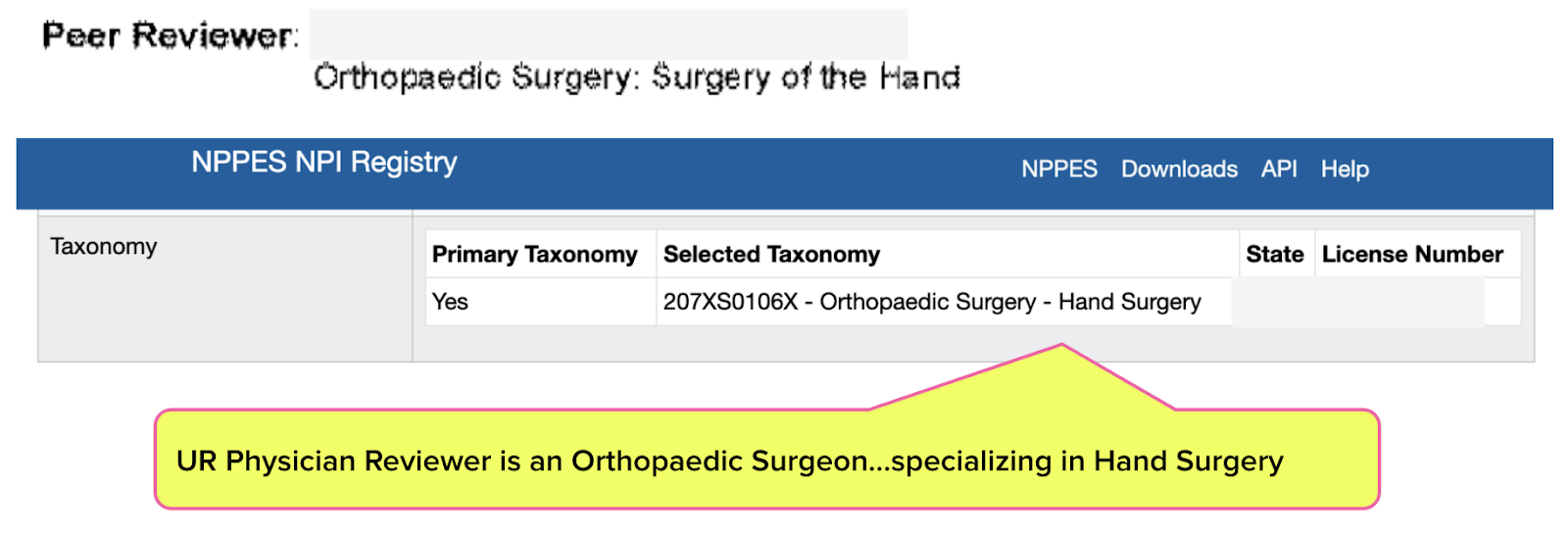
UR physician #2 approved RFA #2 requesting carpal tunnel surgery. Perhaps significantly, UR physician #2 was an expert in — wait for it — hand surgery.
UR Chaos
As e-billing nerds and not physicians, we cannot comment on the actual medical necessity or appropriateness of any given course of treatment. Nor can we comment on the thoroughness of the medical documentation submitted with an RFA.
In this instance, we can however point out that RFA #1 and RFA #2 contained precisely the same medical documentation. For a URO to so drastically and — it can be argued — seemingly arbitrarily flip a decision that could profoundly affect someone’s life and livelihood is unsettling.
This time, the injured worker won out because their treating physician persevered. But when the machinations of UR remain as opaque, inconsistent, and indecipherable as they currently can be sometimes, a single win is little consolation.
Submit RFAs in 30 seconds and automatically track UR decisions with daisyAuth. Request a demo below!
GET DAISYAUTH
DaisyBill provides content as an insightful service to its readers and clients. It does not offer legal advice and cannot guarantee the accuracy or suitability of its content for a particular purpose.



.gif)


