CA: Med-Legal Makes More Financial Sense Than Treatment
.gif)
California physicians must come to terms with an uncomfortable fact: financially, a physician’s time is much better spent conducting Medical-Legal evaluations than actually treating injured workers.
Data from over 126,000 Medical-Legal bills and 340,000 medical treatment bills for dates of service in 2023 reveal:
- The average reimbursement for the most commonly billed Medical-Legal evaluation (a Comprehensive Evaluation, billing code ML201) was over $3,600.
- The average reimbursement for the most commonly billed medical Evaluation and Management (E/M) service (billing code CPT 99214) was $156.
The math is horrifyingly simple: To earn $3,600, a treating physician must conduct 24 E/M visits. But to conduct those E/M visits, the physician incurs far greater treatment and administrative expenses than a Medical-Legal evaluator incurs to perform a single evaluation.
Moreover, California law offers relatively little payment protection to treating physicians denied reimbursement, compared with the robust protections for Medical-Legal evaluators.
Below, we publish the reimbursement data from all 126,000 Medical-Legal bills submitted through our system for 2023 dates of service. Every provider treating injured workers should ask themselves why they continue to participate in a rigged system that clearly devalues their services.
Medical-Legal Services: A Rational Choice for CA Physicians
It is a damning reflection on the overall state of workers’ comp in California, but there’s no denying that offering Medical-Legal services is a boon to the financial health of a practice.
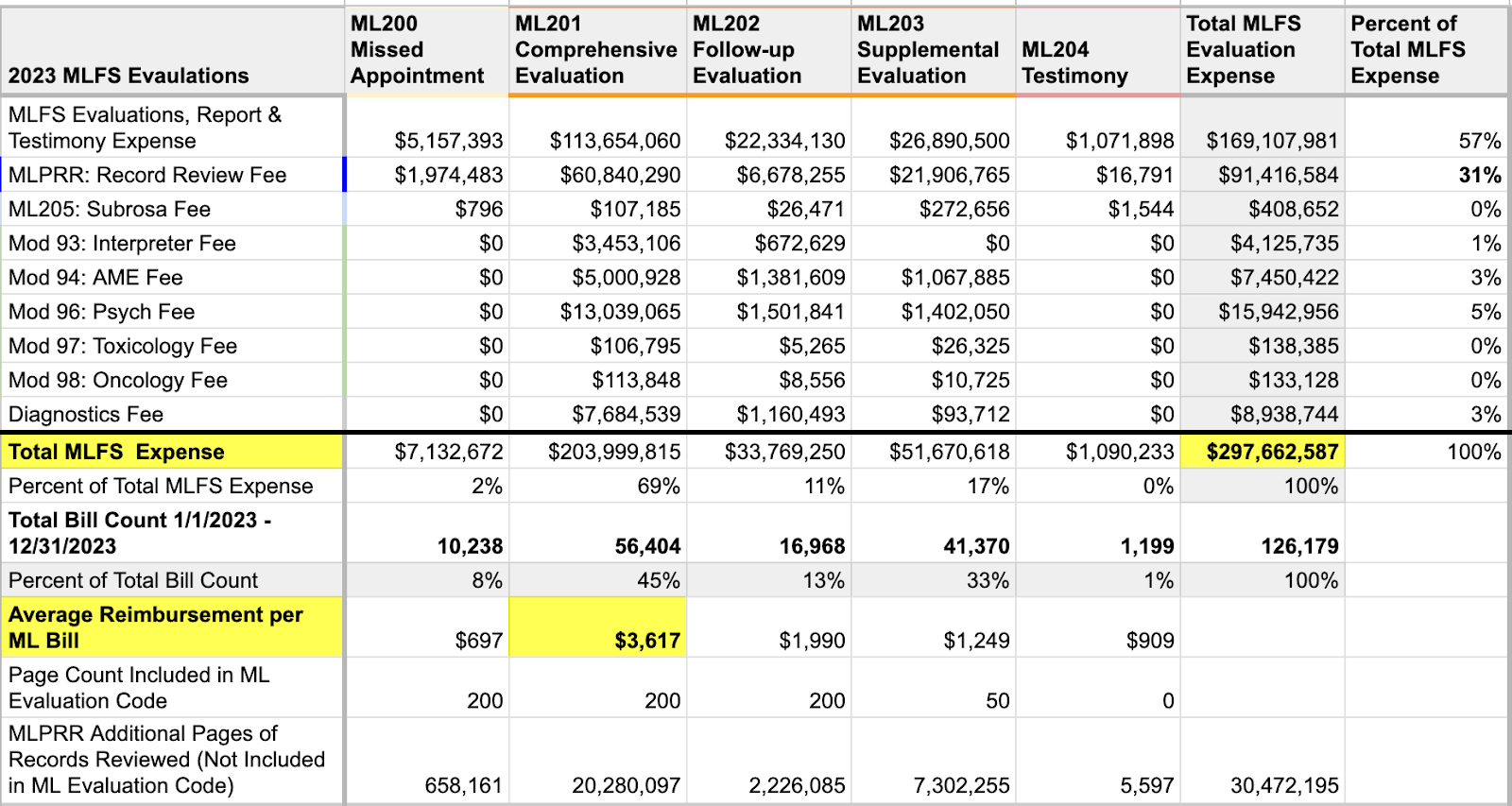
The daisyBill reimbursement data below shows the amount due for reported Medical-Legal evaluations during 2023.
The most common evaluation performed is the Comprehensive Evaluation (ML201), which reimburses an average of $3,617. As noted below, a Medical-Legal evaluator can also expect to provide additional evaluations beyond the Comprehensive Evaluation; 28% of Medical-Legal expenses represented Follow-Up Evaluations (11%) and Supplemental Evaluations (17%).
And of course, fees for medical record review (MLPRR) continue to astound, with over $91 million billed in 2023 — representing 31% of total Medical-Legal expenses.
The Financial Risk of Workers’ Comp Treatment
Various factors make medical treatment for injured workers a poor financial proposition for physicians, leading many to avoid workers’ comp altogether. Those factors include:
- Burdensome billing requirements create opportunities for claims administrators to refuse payment improperly
- A payer-friendly payment appeals process rife with loopholes for claims administrators
- Lax enforcement of payment laws and regulations, leading to rampant (and costly) non-compliance by claims administrators
- Preferred Provider Organization (PPO) discount reimbursement agreements, which physicians sign under threat of removal from Medical Provider Networks (MPNs) — only to see their contractual reimbursement rates leased to dozens of claims administrators, bill review entities, and other vendors
Data from daisyBill show that in 2023, treating providers were collectively paid at just 84% of the reimbursement rates established by California Official Medical Fee Schedules (OMFS) — without factoring in improper payment denials.
Moreover, California law offers far greater payment protection to Medical-Legal evaluators. A Medical-Legal evaluator improperly denied payment may immediately demand a hearing before the Workers’ Compensation Appeals Board (WCAB), which will likely award the evaluator penalty, interest, and attorney fees.
California affords no similar protections to treating physicians denied reimbursement, who must pay $150 to file a lien, pay someone to represent them at the lien hearings, and potentially wait years for the case in chief to settle.
Having recently attended the California Applicants’ Attorneys Association (CAAA) January 2024 convention, daisyBill representatives came away with one clear message: California’s choice to restrict injured workers' access to care has made medical and liability disputes inevitable.
With regard to workers’ comp, California’s physicians have two options: risk taking a loss on the medical treatment of injured workers, or guarantee increased revenue by conducting Medical-Legal services.
Med-Legal billing takes specialized expertise. daisyCollect pros use our advanced software (and experience) to protect your practice. Learn more below:
LEARN MORE
DaisyBill provides content as an insightful service to its readers and clients. It does not offer legal advice and cannot guarantee the accuracy or suitability of its content for a particular purpose.
.gif)

.gif)


.gif)

thanks Daisy Bill for promoting a change to the med-legal fee schedule! Given your effectiveness in getting the DWc to change course ; do you ever consider whether your inflammatory rhetoric helps physicians at all? you can bet this will be sited by payers in pushing for a decrease to MLFs. And you know they aren't going to raise OMFS. You can be sure they won't suggest changes to MPNs or put in rules on discounts. So this comment basically gives the DWC cover to decrease the one bright spot in california WC.
How about some data on how many physicians stop treating? That would help point out the consequences of a discounted fee schedule. Try to help.
Thanks for your comment. While daisyBill is a staunch advocate for providers and injured workers, the role of daisyNews is to report and analyze the facts, and to highlight systemic issues that affect all stakeholders — including the payers.
The disparity between Medical-Legal and medical treatment reimbursements is no “bright spot” for treating providers or California’s injured workers. It is a sign of deep dysfunction that is costing insurers and employers just as surely as it is costing the providers who continue to treat injured workers.
As for the DWC, we would be very poor advocates if we concealed or omitted relevant data out of fear that the state would seek to punish providers further. To stifle our “inflammatory rhetoric” would be a capitulation to the forces currently unraveling the system.
Your suggestion to report on physicians who drop out of workers’ comp treatment is excellent; we have reported on the closures of several practices to injured workers. However, our data, while instructive regarding statewide trends, is limited to the providers in our system. We cannot know how many providers have given up on workers’ comp treatment.
Daisy Bill says the quiet part out loud! As a chiropractor, who is defined as a physician in California Worker's Compensation, I'm completely lost on how I would go about treating an injured worker. Lotta paperwork for, apparently, lousy pay. I haven't treated an injured worker since 2005. I also haven't done a QME since 2005. But, I'm re-upping my QME license because I hear there's demand for more QMEs to be done. $2000+ for an exam and report? Sure! I'll study the physician's guide for that.
But this article underscores what I've been wondering: Who the hell is actually treating injured workers? Because, I'm not. Is anyone?
Your article is spot on. Physicians in the WC arena are financially better off conducting med-legal evaluations -- than actually providing the treatment necessary to "cure or relieve," which is replete with obstacles, shallow shoals, and unseen reefs, all of which can derail a demand for payment.
My facility primarily treated CA injured employees up until 01-01-2005, when the 'hassle factors' associated with treating injured CA employees became too expensive. After 01-01-2005, I spent the next 7 years litigating our outstanding liens before the various district offices of the WCAB, everywhere from San Diego in the South to Redding in the North.
I'm glad I dropped out when I did, as the WC system simply went straight downhill starting in 2013.
For those providers interested in learning more about becoming a QME or AME, be sure to check out CSIMS.ORG -- the California Society of Industrial Medicine and Surgery.
I see where you are coming from however the new MLFS has serious flaws. A basic ML201 pays at $2,015.00, consider the applicant who has multiple injured body parts to examine, evaluate, and rate such as a professional athlete and no medical records to review. Is that even fair? Not to mention that the review companies are arbitrarily denying the ML bills in full, as they can't down code anymore. Or they will pay the evaluation code but deny the MLPRR or visa versa, and Supplemental Reports are always denied, hoping that the providers will submit a SBR to keep the money in their pockets longer. These all now require objections and Petitions/DOR's to now be filed. It's not as easy as you think. Please also keep in mind that a QME who has doesn't perform 8 AME evaluations the prior year must maintain 1/3 percent of his practice for treatment.