SCIF: Inept Utilization Review Delays Care for Injured Worker

We write often about the systemic issues surrounding Utilization Review (UR) in California and the constant struggle of providers to obtain authorization to treat injured workers as they see fit.
But what can get lost in the data is the human element — every improper UR denial or delay means that an injured worker does not receive the treatment they need (or get it soon enough).
Case in point: Genex, the Utilization Review Organization (URO) for the State Compensation Insurance Fund (SCIF), recently added insult to (literal) injury with a nonsensical demand for medical documentation the physician had already faxed to SCIF with the original RFA.
Genex failed to issue a UR decision, citing a lack of information, delaying surgery the treating doctor deemed necessary, and adding even more time to an injured worker's multi-year saga of pain.
We cannot say who dropped the ball: Genex, SCIF, or both.
Undeniably, inadequate oversight of UR by claims administrators fails to disincentivize careless errors, inept decisions, and improper denials of injured workers’ care. In the current system, doctors are forced to comply with stringent RFA requirements — while insurers and their UR organizations suffer zero consequences for failures on their end, which have real consequences for real people.
MD Requests Surgery & Related Treatments
Before an injured worker receives medical treatment of any type, California law requires the physician to submit a Request for Authorization (RFA) to the claims administrator (in this case SCIF) listing the treatments, services, and goods the physician believes are medically necessary. SCIF must respond to the RFA with a Utilization Review (UR) decision approving or denying the recommended treatments.
On July 17, 2023, a daisyBill physician client requested shoulder surgery and other related treatments for an injured worker. The injury was initially reported in 2018 — meaning the injured worker had already endured over three years of this injury without resolution.
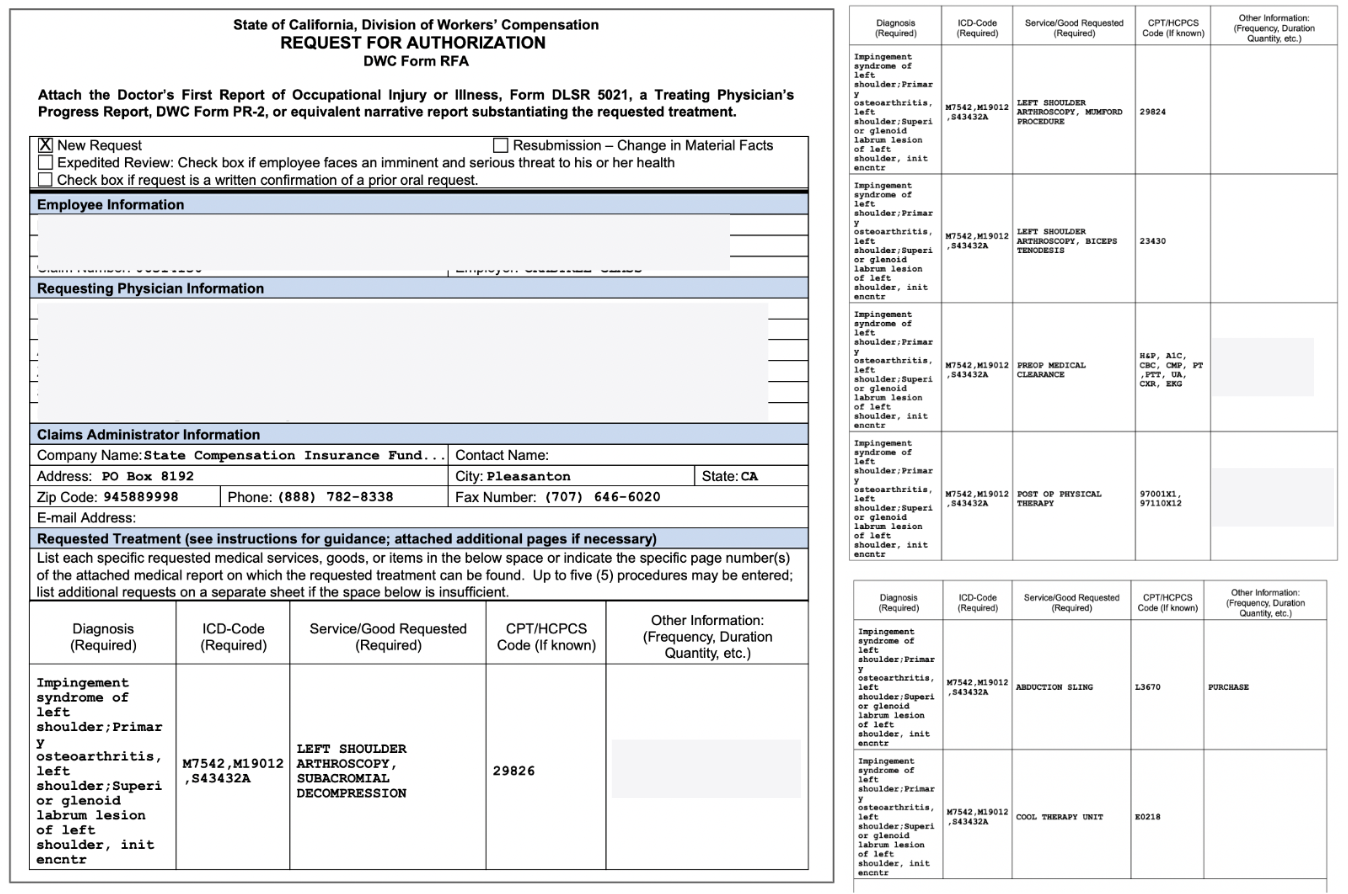
As California regulations require, the doctor faxed SCIF the mandatory RFA detailing all the services and goods related to the surgery, which the physician recommended as medically necessary.
With the RFA form, the doctor also faxed SCIF three medical documents (shown below) supporting the case for the requested surgery, including:
- A recent re-examination report listing the treatments rendered so far, the inadequate results of those treatments on the injury, and the injured workers’ wish to proceed with the surgery recommended by the doctor
- An electrodiagnostic study, and
- MRI results
RFA Fax Receipts Don’t Lie
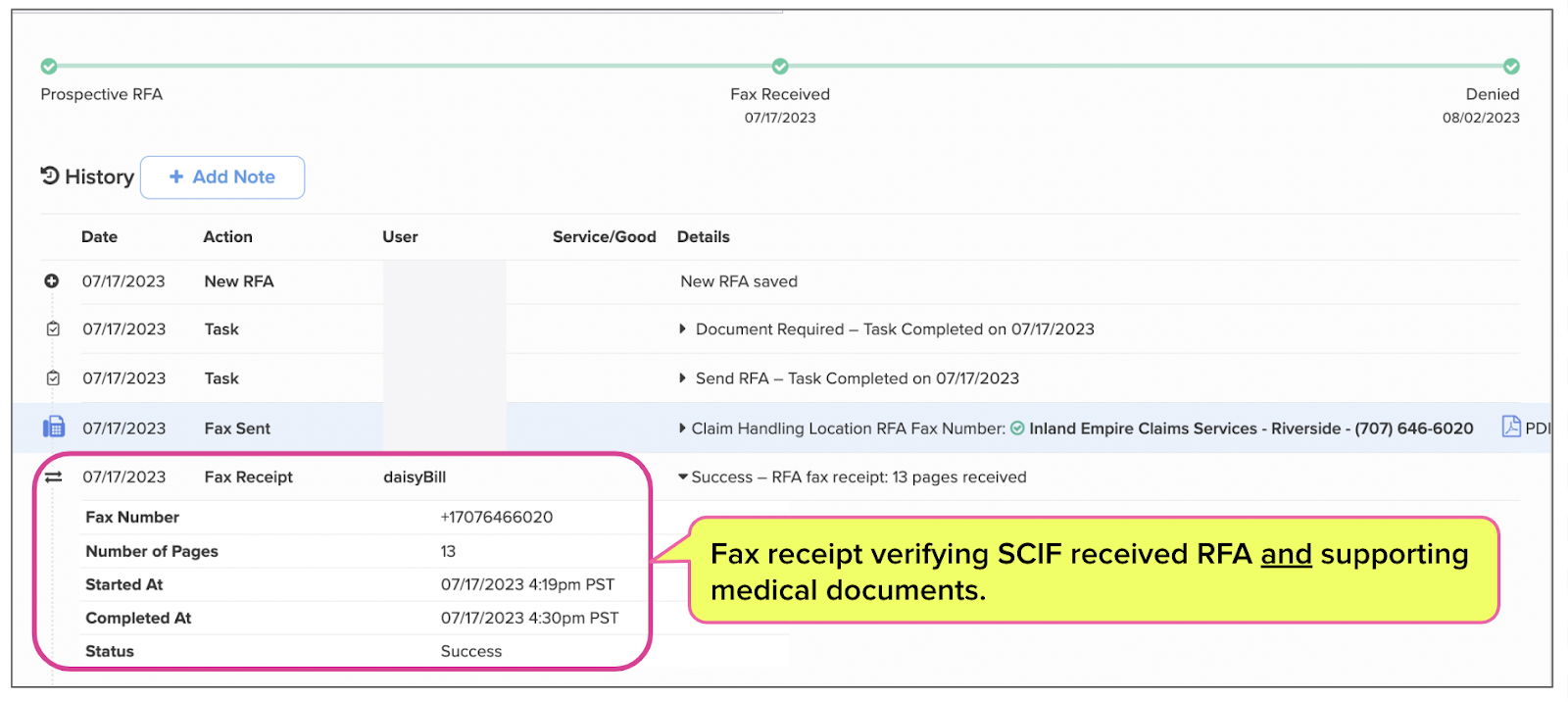
SCIF received the documentation faxed by the physician, as verified by the RFA fax receipt. The screenshot below shows that SCIF received all 13 pages of the RFA at 4:30PM on July 17.
Genex Pumps Brakes, Requests Documentation MD Already Sent
Genex, a Utilization Review Organization used by the State Compensation Insurance Fund (SCIF), responded to the RFA with a letter (shown below) and added insult to (literal) injury by refusing to approve the surgery, citing additional medical documentation was required.
“We have been requested by [SCIF] to perform utilization review to determine if the requested health care services are medically necessary and appropriate…
…the reviewer has determined that additional information is required to make a determination of medical necessity.”
In its letter Genex made a “Request for Additional Information.” However (and infuriatingly), the doctor had faxed SCIF all the information Genex claimed was required to issue a UR decision:
- “Recent subjective and objective information from the requesting provider regarding the claimant’s left shoulder condition.” (Faxed to SCIF with the RFA)
- “Diagnoses, treatments, and responses to treatments for the left shoulder thus far.” (Faxed to SCIF with the RFA)
- “Diagnostic imaging evidence of left shoulder pathology consistent with the requested left shoulder surgical procedure.” (Faxed to SCIF with the RFA)
What’s Next?
Is this delayed care due to Genex's incompetence? SCIF’s bungling of the documentation? In a sense, it doesn’t really matter. What matters is that there are zero consequences for SCIF, Genex, or anyone responsible for this injured worker’s inability to get the surgery deemed necessary by the treating doctor.
All over California, UR organizations operate in an environment in which it is arguably safer to deny or delay care first and ask questions later. If the UR organization errs on the side of approving too much care, the insurer client loses money — presumably a bad thing. But if the UR organization errs on the side of approving too little care…no one suffers except the injured worker.
What do the doctor and injured worker do next?
Should the doctor spend even more administrative resources to fax SCIF the same information again and hope that SCIF and Genex process it competently this time? Will SCIF and/or Genex find another reason to delay or deny surgery? How long will the injured worker wait for surgery? Answers: Only SCIF knows.
Meanwhile, a man hurt at work years ago waits. And waits. And waits — for a UR system that always defaults to the insurer’s advantage, no matter the cost to the injured worker or their employer.
Authorization is the first hurdle in the workers’ comp obstacle course. Enjoy 30-second RFA submission and automatically tracked UR decisions with daisyAuth — request a demo below!
GET DAISYAUTH DEMO
DaisyBill provides content as an insightful service to its readers and clients. It does not offer legal advice and cannot guarantee the accuracy or suitability of its content for a particular purpose.






.gif)


SCIF sucks. UR doctors should be held liable for any harm in patients for denying and delaying care. Leadership at UR companies and insurers should be criminally liable as well